Investigating the Potential Double-Edged Score of Immigration-Related Stress, Discrimination, and Mental Health Access
1. Investigating the Potential Double-Edged Score of Immigration-Related Stress, Discrimination, and Mental Health Access
2. The Health Belief Model and the Potential Roles of Discrimination and Immigration Stress
3. Purpose
The current study sought to quantitatively examine the potential dual roles of discrimination and immigration-related on mental health care seeking. This represents a novel step in examining the potential indirect effects of discrimination and immigration-related stress on mental health care seeking. This is an important step, given prior work indicating that discrimination and immigration-related stress may impede care seeking. Thus, taken together, both discrimination and immigration-related stress may produce conflicting direct and indirect effects on care seeking. To test these hypotheses, the study first examined the direct effects of both factors in potentially reducing care seeking and, subsequently, care utilization. Second, it examined the indirect effects of both factors, with PTSD and depression symptoms as potential mediators. It was hypothesized that both discrimination and immigration-related stress would have negative direct effects on mental health care seeking and care utilization. It was further hypothesized that both discrimination and immigration-related stress would evidence positive indirect effects on care seeking and care utilization with PTSD and depression symptoms as mediators. Specifically, discrimination and immigration-related stress would have positive direct effects on depression and PTSD symptoms. Depression and PTSD symptoms would, in turn, have positive direct effects on care seeking and care utilization.
4. Materials and Methods
4.1. Participants
4.2. Procedure
Participants were recruited separately through phone and internet surveys. For the phone surveys, participants were recruited through multiple local community agencies that served Latinx populations. Participants were also recruited via respondent-driven sampling, in which existing participants were offered incentives for recruiting additional participants (USD 10 gift card for each participant recruited). Prior participants were not informed as to who completed the survey to preserve the confidentiality of participation. Recruitment for the phone survey occurred from November 2020 to August 2021. Recruitment for the internet survey occurred through a university extension agency, which provides education and resources to the local community. Recruitment for the internet wave occurred from January to April 2022. In both cases, surveys were completed as a larger study focusing on COVID-19, stress exposure, mental health, and healthcare access. In both internet and phone surveys, participants were able to complete the study in either English or Spanish. These procedures were approved by the Institutional Review Board (IRB) at the University of Nebraska-Lincoln
4.3. Measures
4.3.1. Discrimination
4.3.2. Immigration-Related Stress
4.3.3. Post-Traumatic Stress Disorder (PTSD)
4.3.4. Depression
4.3.5. Mental Health Access
Mental health access was measured using two items. The first asked participants if they had sought services since the COVID-19 pandemic began but were unable to receive them. The second asked if participants were currently receiving services. These two items, therefore, represent unsuccessful attempts to receive care and current mental health use, respectively. Participants answered either “yes” or “no”, which were then dichotomously coded as “1” and “0”, respectively. As part of exploratory follow-up questions, participants who indicated they had been unable to receive services were asked to identify barriers that prevented them from receiving care.
4.3.6. Demographics
Participants also completed items regarding gender, age, U.S. nativity/country of origin, and education.
4.4. Data Analyses
5. Results
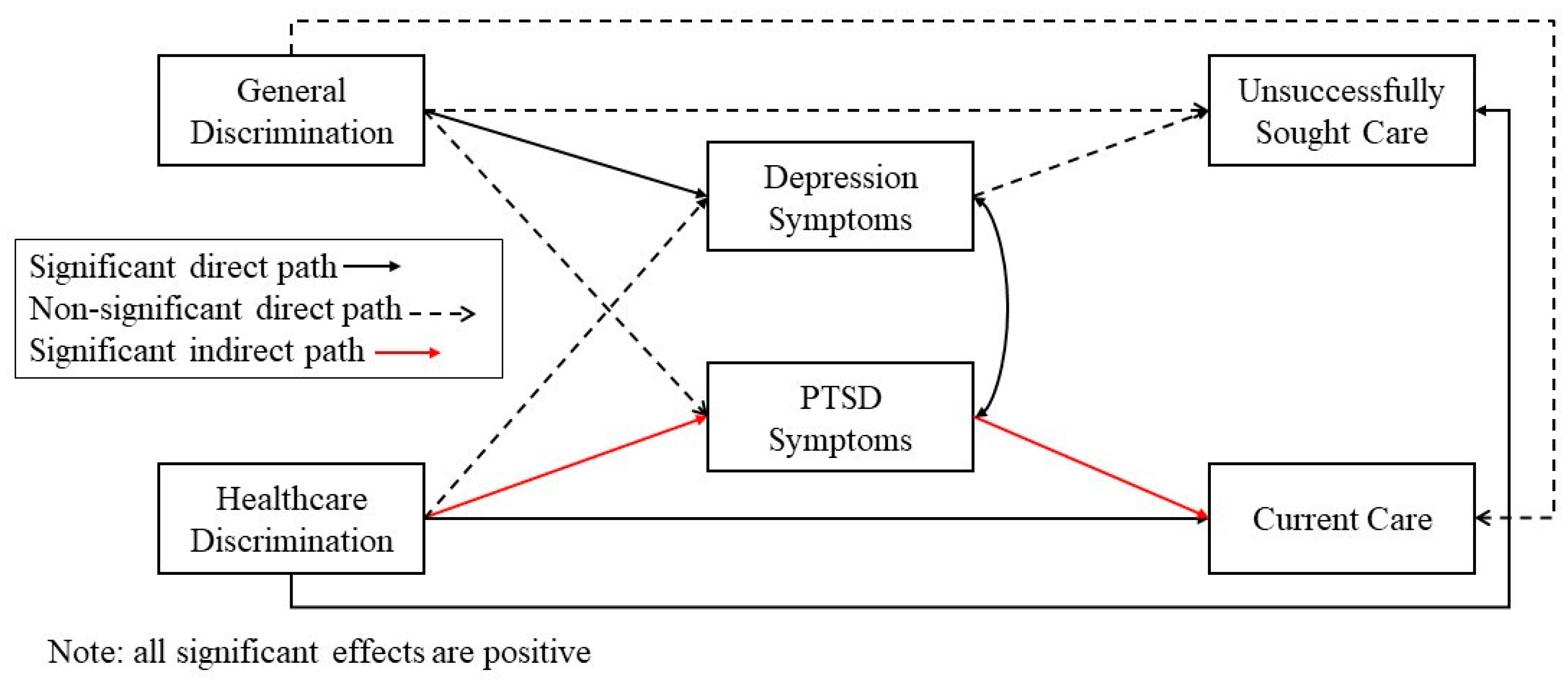
5.1. Discrimination as a Predictor of PTSD and Depression
5.2. Immigration Stress as a Predictor of PTSD and Depression
In the immigration stress model, immigration stress positively predicted PTSD symptoms, b = 0.12, 95% CI = 0.05, 0.18, but was not associated with depression symptoms, b = 0.004, 95% CI = −0.10, 0.10.
5.3. Direct Effects on Mental Health Access Variables
PTSD and Depression Symptoms as Predictors
In the discrimination model, PTSD symptoms were positively associated with having unsuccessfully sought mental health services, aOR = 1.18, b = 0.16, 95% CI = 0.03, 0.38, but depression symptoms were not significantly associated with having unsuccessfully sought services, b = −0.03, 95% CI = −0.18, 0.09. PTSD symptoms were also positively associated with currently receiving care, aOR = 1.16, b = 0.15, 95% CI = 0.01, 0.34. Depression symptoms were not significantly associated with currently receiving mental health services, b = 0.08, 95% CI = −0.06, 0.23. These results did not significantly differ in the immigration stress model.
5.4. Discrimination Variables as Predictors of Access Variables
General discrimination was not associated with either unsuccessfully seeking or currently receiving mental health services (confidence intervals include zero). Discrimination in healthcare settings was positively associated with currently receiving mental health services, aOR = 1.11, b = 0.10, 95% CI = 0.04, 0.21. Discrimination in healthcare settings was not associated with unsuccessfully seeking mental health services, aOR = 1.09, b = 0.09, 95% CI = −0.004, 0.19.
5.5. Immigration Stress as a Predictor of Access Variables
Immigration stress did not predict either currently receiving, aOR = 0.99, b = −0.01, 95% CI = −0.08, 0.06, or unsuccessfully seeking mental health services, aOR = 1.03, b = 0.03, 95% CI = −0.03, 0.10.
5.6. Indirect Effects with Symptomology as Mediators
Because the direct effects of discrimination on PTSD and PTSD on both mental health service access variables were significant, their resulting indirect effects were tested. A similar pattern was also observed for immigration stress with resulting indirect effects. The indirect effect of discrimination on unsuccessfully seeking care with PTSD as a mediator was significant and positive, b = 0.02, 95% CI = 0.01, 0.07. The indirect effect of discrimination on currently receiving care with PTSD as a mediator was also significant and positive, b = 0.02, 95% CI = 0.001, 0.05. The indirect effect of immigration stress on unsuccessfully seeking care with PTSD as a mediator was also significant, b = 0.11, 95% CI = 0.04, 0.19. The indirect effect on currently receiving care was also significant, b = 0.09, 95% CI = 0.02, 0.18.
6. Discussion
The current study examined the potential double-edged sword of discrimination and immigration-related stress. Specifically, the study examined the potential for two opposing effects of discrimination and immigration-related stress on care access: a direct pathway with a lower likelihood of seeking care and an indirect pathway with symptoms as a mediator and a greater likelihood of seeking care. Results testing these hypotheses were mixed. Specifically, general discrimination was only associated with depression symptoms but not PTSD. Conversely, healthcare discrimination and immigration stress were only associated with PTSD, but not depression. Further, discrimination in healthcare settings was associated with currently receiving care, but in the opposite direction than was anticipated. In fact, experiencing discrimination in healthcare settings was associated with higher odds of currently receiving care. General discrimination and immigration-related stress were not directly associated with either help-seeking variable.
In addition to novel findings with the indirect effects of discrimination and immigration-related stress via PTSD, the current study did not support the direct effects of discrimination and immigration-related stress on care seeking. In fact, discrimination in healthcare settings was associated with a higher likelihood of having sought care. This directly conflicts with the Health Belief Model, especially given that discrimination in healthcare was associated with greater care access and seeking. One potential reason for the positive effect of healthcare discrimination on currently receiving care may be related to the cross-sectional nature of this study. Specifically, contact with the mental healthcare system or other referring healthcare systems may produce experiences of discrimination. Thus, those who access care may also be more likely to experience discrimination, which may, in turn, lead to worse PTSD symptomology. Longitudinal research is needed to explicate these relations fully. However, the pattern from the current cross-sectional data may reflect an underlying bidirectional relation in which PTSD increases the likelihood of seeking or receiving care, and contact with the healthcare system results in discrimination, which then worsens PTSD symptomology, leading to an increased need for care. Instead of a double-edged sword, healthcare discrimination may place some in a double bind where the system intended to help alleviate symptoms may worsen these symptoms when discrimination is present. These findings offer potential insights for future areas of inquiry, especially as they relate to the longitudinal roles of discrimination and immigration-related stress on care seeking. It further raises questions regarding the timing of such effects.
7. Limitations and Future Directions
The current study should be considered in the context of multiple limitations. First, the lack of longitudinal data makes it difficult to disentangle the effects of discrimination on healthcare access and to test mediation fully. Second, the study’s convenience sample may limit generalization to other Latinx populations. While the inclusion of a sample recruited outside of any major metropolitan areas may extend the literature, healthcare systems may differ significantly in these areas, including the extent to which people experience discrimination and other available resources. Relatedly, the sample includes primarily cisgender women, and the sample size was insufficient to test gender differences across the effects examined here. Given gender differences in both symptomology and help seeking, results may differ for cisgender men and trans or gender-diverse populations. However, the current results point to potentially fruitful areas of investigation, including longitudinal examination of discrimination, healthcare access, and help-seeking behavior. Future studies should examine different timescales over which discrimination and immigration-related stress predict help seeking. For example, examining whether experiencing discrimination in healthcare settings results in reduced help-seeking attitudes or behaviors over shorter (e.g., days) and longer (e.g., months or days) time intervals. The current study, combined with prior data, indicates that such investigations may shed important light and nuance onto the role of discrimination for Latinx populations in the U.S. Additionally, these results should be examined in different geographical contexts, as they may differ in contexts depending on how welcoming the community is to immigrants and the availability of services.
8. Conclusions
The current study suggests that discrimination in healthcare settings and immigration-related stress may increase PTSD symptoms, which in turn may prompt attempts to access care. The same effects were not present for depression symptoms. This offers new insights into the unique role of PTSD symptoms as consequences of stressors among Latinx populations and immigrants in particular. This novel and somewhat counterintuitive contribution indicates that both discrimination and immigration-related stress may indirectly increase service seeking because both may increase PTSD symptoms.
Author Contributions
Conceptualization, A.R.A., S.R., S.M.E.G. and L.M.A.; methodology, A.R.A.; validation, A.R.A., K.E. and S.R.; formal analysis, A.R.A.; investigation, A.R.A.; resources, A.R.A.; data curation, S.R., K.E. and A.R.A.; writing—original draft preparation, A.R.A. and K.E.; writing—review and editing, A.R.A. and K.E.; visualization, A.R.A.; supervision, A.R.A.; project administration, S.R., L.M.A. and S.M.E.G.; funding acquisition, A.R.A. All authors have read and agreed to the published version of the manuscript.
Funding
Research was funded by the Office of Research and Economic Development at the University of Nebraska-Lincoln.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki and approved by the Institutional Review Board of the University of Nebraska-Lincoln (protocol number 20553 and initially approved 14 September 2020).
Informed Consent Statement
Informed consent was obtained from all participants involved in the study.
Data Availability Statement
Data are not available for sharing due to privacy concerns of participants. Additional data summaries may be provided upon request.
Acknowledgments
We would like to thank our community partners, El Centro de las Américas, for completing this study.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Andrews, A.R., III; Haws, J.K.; Acosta, L.M.; Acosta Canchila, M.N.; Carlo, G.; Grant, K.M.; Ramos, A.K. Combinatorial effects of discrimination, legal status fears, adverse childhood experiences, and harsh working conditions among Latino migrant farmworkers: Testing learned helplessness hypotheses. J. Latinx Psychol. 2020, 8, 179–201. [Google Scholar] [CrossRef] [PubMed]
- Bernard, D.L.; Smith, Q.; Lanier, P. Racial discrimination and other adverse childhood experiences as risk factors for internalizing mental health concerns among Black youth. J. Trauma. Stress. 2021, 35, 473–483. [Google Scholar] [CrossRef] [PubMed]
- Budhwani, H.; Hearld, K.R.; Chavez-Yenter, D. Depression in Racial and Ethnic Minorities: The Impact of Nativity and Discrimination. J. Racial Ethn. Health Disparities 2015, 2, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Coffman, M.J.; Norton, C.K. Demands of Immigration, Health Literacy, and Depression in Recent Latino Immigrants. Home Health Care Manag. Pract. 2010, 22, 116–122. [Google Scholar] [CrossRef]
- Dang, B.N.; Giordano, T.P.; Kim, J.H. Sociocultural and structural barriers to care among undocumented Latino immigrants with HIV infection. J. Immigr. Minor. Health 2012, 14, 124–131. [Google Scholar] [CrossRef] [PubMed]
- Ortega, A.N.; Fang, H.; Perez, V.H.; Rizzo, J.A.; Carter-Pokras, O.; Wallace, S.P.; Gelberg, L. Health Care Access, Use of Services, and Experiences Among Undocumented Mexicans and Other Latinos. Arch. Intern. Med. 2007, 167, 2354–2360. [Google Scholar] [CrossRef]
- Abraham, C.; Sheeran, P. Predicting Health Behaviour: Research and Practice with Social Cognition Models; Open University Press Berkshire, 2015; pp. 30–55. Available online: https://books.google.com/books?hl=en&lr=&id=pMkvEAAAQBAJ&oi=fnd&pg=PA30&dq=health+belief+model&ots=eXXFA6jrLC&sig=4zFKlDJvM93OJlFAt8xN5Z0RUBc (accessed on 28 January 2024).
- Champion, V.L.; Skinner, C.S. The health belief model. Health Behav. Health Educ. Theory Res. Pract. 2008, 4, 45–65. [Google Scholar]
- Brooks Holliday, S.; Dubowitz, T.; Haas, A.; Ghosh-Dastidar, B.; DeSantis, A.; Troxel, W.M. The association between discrimination and PTSD in African Americans: Exploring the role of gender. Ethn. Health 2020, 25, 717–731. [Google Scholar] [CrossRef]
- Williams, M.T.; Printz, D.; DeLapp, R.C. Assessing racial trauma with the Trauma Symptoms of Discrimination Scale. Psychol. Violence 2018, 8, 735. [Google Scholar] [CrossRef]
- Henshaw, E.J.; Freedman-Doan, C.R. Conceptualizing mental health care utilization using the health belief model. Clin. Psychol. Sci. Pract. 2009, 16, 420. [Google Scholar] [CrossRef]
- Hunt, J.; Sullivan, G.; Chavira, D.A.; Stein, M.B.; Craske, M.G.; Golinelli, D.; Roy-Byrne, P.P.; Sherbourne, C.D. Race and beliefs about mental health treatment among anxious primary care patients. J. Nerv. Ment. Dis. 2013, 201, 188–195. [Google Scholar] [CrossRef]
- Nobiling, B.D.; Maykrantz, S.A. Exploring Perceptions about and Behaviors Related to Mental Illness and Mental Health Service Utilization among College Students Using the Health Belief Model (HBM). Am. J. Health Educ. 2017, 48, 306–319. [Google Scholar] [CrossRef]
- O’Connor, P.J.; Martin, B.; Weeks, C.S.; Ong, L. Factors that influence young people’s mental health help-seeking behaviour: A study based on the Health Belief Model. J. Adv. Nurs. 2014, 70, 2577–2587. [Google Scholar] [CrossRef] [PubMed]
- Langley, E.L.; Wootton, B.M.; Grieve, R. The Utility of the Health Belief Model Variables in Predicting Help-Seeking Intention for Anxiety Disorders. Aust. Psychol. 2018, 53, 291–301. [Google Scholar] [CrossRef]
- Canchila, M.; Reyes, S.; Estrada Gonzalez, S.M.; Dominguez, V.; Acosta, L.M.; Guerra, R.; Pulido, C.; Caicedo, O.; Andrews, A.R. The role of discrimination and vaccine distrust in vaccine uptake among Latines in the Midwest. Behav. Ther. 2022. Available online: https://psycnet.apa.org/record/2023-15394-001 (accessed on 28 January 2024).
- Hacker, K.; Anies, M.E.; Folb, B.; Zallman, L. Barriers to health care for undocumented immigrants: A literature review. RMHP 2015, 8, 175–183. [Google Scholar] [CrossRef] [PubMed]
- Asad, A.L. Latinos’ deportation fears by citizenship and legal status, 2007 to 2018. Proc. Natl. Acad. Sci. USA 2020, 117, 8836–8844. [Google Scholar] [CrossRef]
- Cox, R.B.; Lin, H.; Cartagena, M.J.L.; Greder, K.A.; Larzelere, R.E.; Washburn, I.J.; Sahbaz, S. Validation of the Family Fear of Deportation Scale for youth. Fam. Relat. 2023, 72, 734–754. [Google Scholar] [CrossRef]
- Rayburn, A.D.; McWey, L.M.; Gonzales-Backen, M.A. Living Under the Shadows: Experiences of Latino Immigrant Families at Risk for Deportation. Fam. Relat. 2021, 70, 359–373. [Google Scholar] [CrossRef]
- Brabeck, K.M.; Cardoso, J.B.; Chen, T.; Bjugstad, A.; Capps, R.; Capoverde, E.; Trull, A. Discrimination and PTSD among Latinx immigrant youth: The moderating effects of gender. Psychol. Trauma: Theory Res. Pract. Policy 2022, 14, 11. [Google Scholar] [CrossRef]
- Cobb, C.L.; Xie, D.; Meca, A.; Schwartz, S.J. Acculturation, discrimination, and depression among unauthorized Latinos/as in the United States. Cult. Divers. Ethn. Minor. Psychol. 2017, 23, 258–268. [Google Scholar] [CrossRef] [PubMed]
- Torres, L.; Ong, A.D. A daily diary investigation of Latino ethnic identity, discrimination, and depression. Cult. Divers. Ethn. Minor. Psychol. 2010, 16, 561. [Google Scholar] [CrossRef] [PubMed]
- Pérez, D.J.; Fortuna, L.; Alegría, M. Prevalence and correlates of everyday discrimination among U.S. Latinos. J. Community Psychol. 2008, 36, 421–433. [Google Scholar] [CrossRef]
- Peek, M.E.; Nunez-Smith, M.; Drum, M.; Lewis, T.T. Adapting the Everyday Discrimination Scale to Medical Settings: Reliability and Validity Testing in a Sample of African American Patients. Ethn. Dis. 2011, 21, 502–509. [Google Scholar] [PubMed]
- Stucky, B.D.; Gottfredson, N.C.; Panter, A.T.; Daye, C.E.; Allen, W.R.; Wightman, L.F. An item factor analysis and item response theory-based revision of the Everyday Discrimination Scale. Cult. Divers. Ethn. Minor. Psychol. 2011, 17, 175. [Google Scholar] [CrossRef] [PubMed]
- Taylor, R.J.; Forsythe-Brown, I.; Mouzon, D.M.; Keith, V.M.; Chae, D.H.; Chatters, L.M. Prevalence and correlates of everyday discrimination among black Caribbeans in the United States: The impact of nativity and country of origin. Ethn. Health 2019, 24, 463–483. [Google Scholar] [CrossRef] [PubMed]
- Sternberg, R.M.; Nápoles, A.M.; Gregorich, S.; Paul, S.; Lee, K.A.; Stewart, A.L. Development of the Stress of Immigration Survey (SOIS): A Field Test among Mexican Immigrant Women. Fam. Community Health 2016, 39, 40–52. [Google Scholar] [CrossRef]
- Blevins, C.A.; Weathers, F.W.; Davis, M.T.; Witte, T.K.; Domino, J.L. The Posttraumatic Stress Disorder Checklist for DSM-5 (PCL-5): Development and Initial Psychometric Evaluation. J. Trauma. Stress. 2015, 28, 489–498. [Google Scholar] [CrossRef]
- Miller-Graff, L.E.; Guzman, J.C.; Hare, T. Psychometric Properties of the CES-D, PCL-5, and DERS in a Honduran Adult Sample. Psychol. Test. Adapt. Dev. 2023, 4, 300–309. [Google Scholar] [CrossRef]
- Martínez-Levy, G.A.; Bermúdez-Gómez, J.; Merlín-García, I.; Flores-Torres, R.P.; Nani, A.; Cruz-Fuentes, C.S.; Briones-Velasco, M.; Ortiz-León, S.; Mendoza-Velásquez, J. After a disaster: Validation of PTSD checklist for DSM-5 and the four- and eight-item abbreviated versions in mental health service users. Psychiatry Res. 2021, 305, 114197. [Google Scholar] [CrossRef] [PubMed]
- Kroenke, K.; Spitzer, R.L. The PHQ-9: A new depression diagnostic and severity measure. Psychiatr. Ann. 2002, 32, 509–515. [Google Scholar] [CrossRef]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B. The Phq-9. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef] [PubMed]
- Wulsin, L.; Somoza, E.; Heck, J. The Feasibility of Using the Spanish PHQ-9 to Screen for Depression in Primary Care in Honduras. Prim. Care Companion J. Clin. Psychiatry 2002, 4, 191–195. [Google Scholar] [CrossRef] [PubMed]
- Zhong, Q.; Gelaye, B.; Fann, J.R.; Sanchez, S.E.; Williams, M.A. Cross-cultural validity of the Spanish version of PHQ-9 among pregnant Peruvian women: A Rasch item response theory analysis. J. Affect. Disord. 2014, 158, 148–153. [Google Scholar] [CrossRef] [PubMed]
- Kroenke, K.; Strine, T.W.; Spitzer, R.L.; Williams, J.B.; Berry, J.T.; Mokdad, A.H. The PHQ-8 as a measure of current depression in the general population. J. Affect. Disord. 2009, 114, 163–173. [Google Scholar] [CrossRef]
- Enders, C.K.; Bandalos, D.L. The relative performance of full information maximum likelihood estimation for missing data in structural equation models. Struct. Equ. Model. 2001, 8, 430–457. [Google Scholar] [CrossRef]
- McClendon, J.; Dean, K.E.; Galovski, T. Addressing Diversity in PTSD Treatment: Disparities in Treatment Engagement and Outcome Among Patients of Color. Curr. Treat. Options Psych. 2020, 7, 275–290. [Google Scholar] [CrossRef]
Figure 1.
Path model of direct and indirect effects of discrimination on mental health access.
Figure 1.
Path model of direct and indirect effects of discrimination on mental health access.
Figure 2.
Path model of direct and indirect effects of immigration stress on mental health access.
Figure 2.
Path model of direct and indirect effects of immigration stress on mental health access.
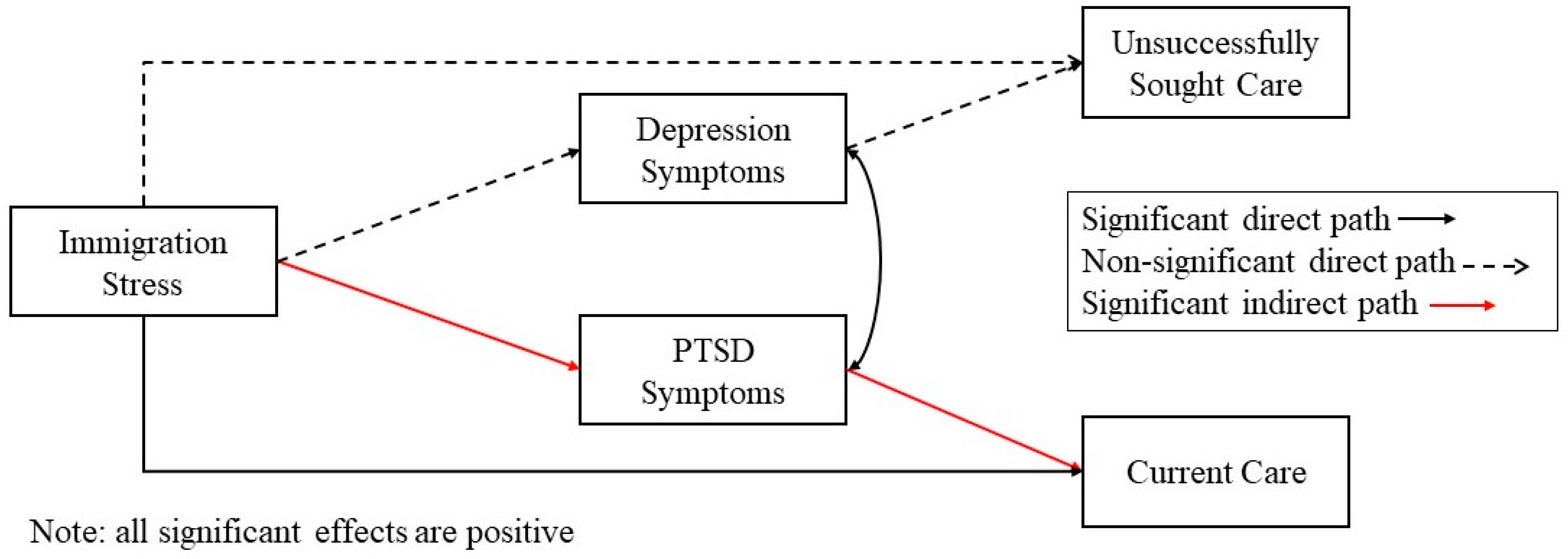
Table 1.
Demographic and descriptive information.
Table 1.
Demographic and descriptive information.
| n (%) | ||
|---|---|---|
| Gender | ||
| Cisgender women | 165 (70.2) | |
| Cisgender men | 65 (27.7) | |
| Transgender men | 1 (0.4) | |
| Born outside the U.S. | 197 (83.8) | |
| Mexico | 91 (38.7) | |
| Caribbean | 39 (16.6) | |
| Central America | 45 (19.1) | |
| South America | 23 (9.8) | |
| Education | ||
| Less than high school | 50 (21.3) | |
| Completed high school | 86 (36.6) | |
| Some college or higher | 92 (39.1) | |
| Unsuccessfully sought mental health care | 21 (8.9) | |
| Currently receiving care (yes) | 21 (8.9) | |
| M (SD) | Min-Max | |
| Age | 42.52 (14.21) | 19–82 |
| Annual household income (in USD) | 42,596 (33,963) | 0–200,000 |
| PHQ-8 (depression symptoms) | 7.12 (5.50) | 0–24 |
| Abbreviated PCL-5 (PTSD symptoms) | 2.41 (3.11) | 0–14 |
| Everyday discrimination | 5.26 (4.88) | 0–20 |
| Discrimination in healthcare | 12.09 (2.98) | 4–20 |
| Immigration-related stress | 38.15 (9.21) | 16–58 |
Table 2.
Predictors of mental health access variables.
Table 2.
Predictors of mental health access variables.
| Predictor | Dependent Variables | |
|---|---|---|
| Unsuccessfully Seeking Care | Current Care Utilization | |
| aOR | aOR | |
| Gender | 0.85 | 0.77 |
| Age | 0.78 | 1.10 |
| Everyday discrimination | 1.00 | 1.01 |
| Healthcare discrimination | 1.11 * | 1.09 * |
| Depression symptoms (PHQ-8) | 0.97 | 1.08 |
| PTSD symptoms (PCL) | 1.16 * | 1.18 * |
| Immigration-related stress | 1.03 | 0.99 |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |