COVID | Free Full-Text | A Mediation Model of Self-Efficacy and Depression between Burnout and Alcohol Consumption among Health Workers during the COVID-19 Pandemic
[ad_1]
1. Introduction
To better understand the relationship among work demands, individual resources and their consequences at the emotional and behavioral levels, an analytical model was established in which the COVID-19 pandemic (generalized demand) put health workers under immense stress, leading them to experience burnout (personal demand), with a consequent increase in the probability of consuming alcohol (personal outcome); self-efficacy and depression (a personal resource and a personal lack of resources, respectively) act as mediators of this relationship.
1.1. Job Demands and Resources Model
1.2. Alcohol Consumption
Therefore, the purpose of the present study was to test an analytical model in which the COVID-19 pandemic (generalized demand) has put health workers under immense stress and led them to experience burnout (personal demand), with a consequent increase in the probability of consuming alcohol (personal outcome), where self-efficacy and depression (a personal resource and a personal lack of resources, respectively) mediate the relationship.
2. Materials and Methods
We conducted data collection during the 2nd and 3rd COVID-19 waves in Mexico as a part of a psychoeducational intervention organized by the Mexico City Health Ministry and the Labor Union of the Mexican Social Security Institute. The courses and participation in the cross-sectional study were offered to all affiliated workers, including physicians, nurses, administrators, pharmacists, security workers, etc. throughout the COVID-19 pandemic. Enrollment in the intervention program and taking the survey were both voluntary and anonymous processes. At the beginning of the online survey, the participants gave their consent to start responding. Participants needed to be active workers and to give their consent to participate in the study; they also needed to have an active email account to which the invitation to participate in the research could be sent. No exclusion criteria were established, and the only elimination criteria were incomplete data in the sociodemographic section and more than 20% missing data in the complete survey.
2.1. Participants
2.2. Instruments
The survey was part of a larger applied study on the mental health of health workers with a pilot intervention program aimed at ameliorating the potential distress suffered by health workers during the COVID-19 pandemic. The survey was conceived as a screening tool for the participants to enroll in a series of online free courses. Participation in the online courses and the screening test were completely voluntary and anonymous, and the participants signed an informed consent form before enrolling.
In the current study, we focused on the responses on four scales included in the survey, which were presented to each participant in the same order. In the sociodemographic section, the participants were asked to indicate their gender, age, marital status, educational level and main area of work. Immediately thereafter, the participants were presented with the following psychological scales in the subsequent order:
2.2.1. Burnout Scale
2.2.2. Depression Scale
2.2.3. Self-Efficacy Index
2.2.4. Alcohol Consumption
2.3. Procedure
Before the course videos were presented, a pop-up window asked the participants whether they would be interested in participating in a survey. If the participant agreed to participate, then an informed consent form was displayed. After providing informed consent, the participants could start the survey and could pause or drop out at any time, and the participants had the option to go directly to the online course material instead. When the participants finalized the survey, they received feedback on the results, and if their scores were high, they were shown an informative note directing them to seek psychological services. The participants were redirected to the online courses after they finished the survey. The survey lasted approximately 25 min.
2.4. Data Analyses
3. Results
Two hundred and seventy-nine participants were enrolled in clinical and medical care (53.9%), 1081 were working in administrative positions (28%), 69 were collaborating in clinical and laboratory analyses (1.8%) and 627 worked in general services (e.g., security and IT; 16.3%). Of the total sample, 2884 identified themselves as women (74.8%), and 972 identified as men (25.2%), with an age range from 20 to 66 years old (Mage = 38.29 years; S.D. age = 9.5 years); 1892 reported being single or divorced (49.1%), 1964 were married or in a free union (50.9%), 815 had a secondary level of education (years 7 to 12; 21.1%), 1832 had a bachelor’s diploma (47.5%) and 1209 had a postgraduate degree (medical specialization, master’s and doctoral degrees; 31.4%).
Based on these results, we can partially support the assertion that burnout directly predicts alcohol consumption. Emotional exhaustion and achievement dissatisfaction did not have a direct significant effect on alcohol consumption, and only depersonalization had a significant positive effect on alcohol consumption. Self-efficacy and depression significantly predicted alcohol consumption, and the latter had the greatest effect.
4. Discussion
One limitation of the current study is that random sampling procedures were not used for the survey, which limits the generalizability of the findings. All of the participants voluntarily agreed to complete the survey, which may have led to a self-selection bias. The survey was distributed online, which prevented potential participants with restricted access to electronic infrastructure (e.g., concierges and security guards) from being included.
5. Conclusions
The severe effects of burnout, such as depression and increased alcohol consumption, can be prevented by fostering a sense of self-efficacy. Strengthening a sense of competence and reducing institutional stressors (e.g., providing sufficient work materials and relevant and adequate rest and recreation space) will reduce the probability of engaging in unhealthy coping strategies, such as alcohol consumption, among health workers.
Supplementary Materials
Author Contributions
Conceptualization, A.d.C.D.-E., F.L.S., A.M.P.V. and G.P.H.; data curation, A.d.C.D.-E.; formal analysis, A.d.C.D.-E.; writing—original draft, A.d.C.D.-E. and F.L.S. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
The review of the ethical aspects of the screening test were supervised by the researchers at the Iberoamerican University and the authorities of the Mexico City Ministry of Health and the Mexican Social Security Institute Labor Union in strict adherence to the Helsinki Declaration and the Regulation of the General Health Law on Research for Health for Mexico.
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
Acknowledgments
We thank the staff from the Direction for Training and Self-actualization and Research of the Secretary of Health of Mexico City and the Secretary of Women’s Action of the National Union of Social Security Workers for helping to collect the data. We also thank the Continuing Education Office from the Iberoamerican University for their support in launching the survey on the online platform. We also would like to thank Tonathiu Salcedo for helping upload the questionnaire to the online platform.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Kniffin, K.M.; Narayanan, J.; Anseel, F.; Antonakis, J.; Ashford, S.P.; Bakker, A.B.; Bamberger, P.; Bapuji, H.; Bhave, D.P.; Choi, V.K.; et al. COVID-19 and the workplace: Implications, issues, and insights for future research and action. Am. Psychol. 2021, 76, 63–77. [Google Scholar] [CrossRef]
- Preti, E.; Di Mattei, V.; Perego, G.; Ferrari, F.; Mazzetti, M.; Taranto, P.; Di Pierro, R.; Madeddu, F.; Calati, R. The psychological impact of epidemic and pandemic outbreaks on healthcare workers: Rapid review of the evidence. Curr. Psychiatry Rep. 2020, 22, 22. [Google Scholar] [CrossRef] [PubMed]
- Sultana, A.; Sharma, R.; Hossain, M.M.; Bhattacharya, S.; Purohit, N. Burnout among healthcare providers during COVID-19: Challenges and evidence-based interventions. Indian J. Med. Ethics 2020, 5, 308–311. [Google Scholar] [CrossRef] [PubMed]
- White, E.M.; Wetle, T.F.; Reddy, A.; Baier, R.R. Front-line nursing home staff experiences during the COVID-19 Pandemic. J. Am. Med. Dir. Assoc. 2021, 22, 199–203. [Google Scholar] [CrossRef] [PubMed]
- Young, K.P.; Kolcz, D.L.; O’Sullivan, D.M.; Ferrand, J.; Fried, J.; Robinson, K. Health care workers’ mental health and quality of life during COVID-19: Results from a mid-pandemic, national survey. Psychiatr. Serv. 2021, 72, 122–128. [Google Scholar] [CrossRef]
- Zerden, L.D.S.; Richman, E.L.; Lombardi, B.; Forte, A.B. Frontline, essential, and invisible: The needs of low-wage workers in hospital settings during COVID-19. Workplace Health Saf. 2022, 70, 509–514. [Google Scholar] [CrossRef]
- Tipa, R.O.; Tudose, C.; Pucarea, V.L. Measuring burnout among psychiatric residents using the Oldenburg Burnout Inventory (OLBI) Instrument. J. Med. Life 2019, 12, 354–360. [Google Scholar] [CrossRef]
- Bakker, A.; Demerouti, E.; Schaufeli, W. Dual processes at work in a call centre: An application of the job demands–resources model. Eur. J. Work. Organ. Psychol. 2003, 12, 393–417. [Google Scholar] [CrossRef]
- Demerouti, E.; Bakker, A.B.; Nachreiner, F.; Schaufeli, W.B. The job demands-resources model of burnout. J. Appl. Psychol. 2001, 86, 499–512. [Google Scholar] [CrossRef]
- Bakker, A.B.; Demerouti, E.; Euwema, M.C. Job resources buffer the impact of job demands on burnout. J. Occup. Health Psychol. 2005, 10, 170–180. [Google Scholar] [CrossRef]
- Bakker, A.B.; Demerouti, E. Job demands–resources theory: Taking stock and looking forward. J. Occup. Health Psychol. 2017, 22, 273–285. [Google Scholar] [CrossRef] [PubMed]
- Njim, T.; Mbanga, C.M.; Tindong, M.; Fonkou, S.; Makebe, H.; Toukam, L.; Fondungallah, J.; Fondong, A.; Mulang, I.; Kika, B. Burnout as a correlate of depression among medical students in Cameroon: A cross-sectional study. BMJ Open 2019, 9, e027709. [Google Scholar] [CrossRef]
- Talih, F.; Daher, M.; Daou, D.; Ajaltouni, J. Examining burnout, depression, and attitudes regarding drug use among Lebanese medical students during the 4 years of medical school. Acad. Psychiatry 2018, 42, 288–296. [Google Scholar] [CrossRef] [PubMed]
- Walkiewicz, M.; Tartas, M. Vulnerability of medical students and professionals to extreme work stress: A select review of the literature. Commun. Med. 2017, 14, 181–187. [Google Scholar] [CrossRef] [PubMed]
- Hyman, S.A.; Shotwell, M.S.; Michaels, D.R.; Han, X.; Card, E.B.; Morse, J.L.; Weinger, M.B. A survey evaluating burnout, health status, depression, reported alcohol and substance use, and social support of Anesthesiologists. Anesth. Analg. 2017, 125, 2009–2018. [Google Scholar] [CrossRef]
- Sklar, M.; Ehrhart, M.G.; Aarons, G.A. COVID-related work changes, burnout, and turnover intentions in mental health providers: A moderated mediation analysis. Psychiatr. Rehabil. J. 2021, 44, 219. [Google Scholar] [CrossRef]
- Bandura, A. Self-efficacy mechanism in human agency. Am. Psychol. 1982, 37, 122–147. [Google Scholar] [CrossRef]
- Bandura, A. Social Cognitive Theory of self-regulation. Organ. Behav. Hum. Decis. Process. 1991, 50, 248–287. [Google Scholar] [CrossRef]
- Bandura, A. Cultivate self-efficacy for personal and organizational effectiveness. In Handbook of Principles of Organization Behavior; Locke, E.A., Ed.; Blackwell: Oxford, UK, 2000; pp. 120–135. [Google Scholar]
- Abdelsadig Mohammed, H.; Elamin, S.A.; El-Awaisi, A.; El Hajj, M.S. Use of the job demands-resource model to understand community pharmacists’ burnout during the COVID-19 pandemic. Res. Soc. Adm. Pharm. 2022, 18, 3568–3579. [Google Scholar] [CrossRef]
- Albergo, J.I.; Fernández, M.C.; Zaifrani, L.; Giunta, D.H.; Albergo, L. ¿Cómo afecta la privación de sueño durante una guardia de 24 horas las funciones cognitivas de los residentes de ortopedia y traumatología? [How does sleep deprivation during 24 hours on call duty affect the cognitive performance orthopaedic residents?]. Rev. Esp. Cir. Ortop. Traumatol. 2016, 60, 113–118. [Google Scholar] [CrossRef]
- Dewa, C.; Loong, D.; Bonato, S.; Trojanowski, L.; Rea, M. The relationship between resident burnout and safety-related and acceptability-related quality of healthcare: A systematic literature review. BMC Med. Educ. 2017, 17, 195. [Google Scholar] [CrossRef] [PubMed]
- An, T.W.; Henry, J.K.; Igboechi, O.; Wang, P.; Yerrapragada, A.; Lin, C.A.; Paiement, G.D. How are orthopaedic surgery residencies responding to the COVID-19 pandemic? An assessment of resident experiences in cities of major virus outbreak. J. Am. Acad. Orthop. Surg. 2020, 28, 679–685. [Google Scholar] [CrossRef]
- Barello, S.; Palamenghi, L.; Graffigna, G. Burnout and somatic symptoms among frontline healthcare professionals at the peak of the Italian COVID-19 pandemic. Psychiatry Res. 2020, 290, e113129. [Google Scholar] [CrossRef] [PubMed]
- García-Torres, M.; Aguilar-Castro, J.; García-Méndez, M. Psychological weelbeing and burnout in health care providers during the COVID-19 pandemic [Bienestar psicológico y burnout en personal de salud durante la pandemia de COVID-19]. Escr. Psicol. 2021, 14, 96–106. [Google Scholar] [CrossRef]
- Torres-Muñoz, V. Riesgos y daños en la salud mental del personal sanitario por la atención a pacientes con COVID-19 [Risks and damage to the mental health of health personnel due to the care of patients with COVID-19]. Rev. Mex. Urol. 2020, 80, 1–9. [Google Scholar] [CrossRef]
- Killikelly, C.; Lenferink, L.I.M.; Xie, H.; Maercker, A. Rapid systematic review of psychological symptoms in health care workers COVID-19. J. Loss Trauma 2021, 26, 638–655. [Google Scholar] [CrossRef]
- Robles, R.; Rodríguez, E.; Vega-Ramírez, H.; Álvarez-Icaza, D.; Madrigal, E.; Durand, S.; Astudillo, C.; Becerra, C.; Escamilla, R.; Diaz, D.; et al. Mental health problems among healthcare workers involved with the COVID-19 outbreak. Braz. J. Psychiatry 2020, 43, 494–503. [Google Scholar] [CrossRef]
- Mahase, E. Coronavirus COVID-19 has killed more people than SARS and MERS combined, despite lower case fatality rate. BMJ 2020, 368, m641. [Google Scholar] [CrossRef]
- Pan American Health Organization/World Health Organization. Epidemiological Alert: COVID-19 among Healthcare Workers; Pan American Health Organization: Washington, DC, USA, 2020. [Google Scholar]
- Muñoz del Carpio-Toia, A.; Begazo Muñoz del Carpio, L.; Mayta-Tristan, P.; Alarcón-Yaquetto, D.E.; Málaga, G. Workplace violence against physicians treating COVID-19 patients in Peru: A cross-sectional study. Jt. Comm. J. Qual. Patient Saf. 2021, 47, 637–645. [Google Scholar] [CrossRef] [PubMed]
- Rzymski, P.; Mamzer, H.; Nowicki, M. The main sources and potential effects of COVID-19-related discrimination. In Coronavirus Disease—COVID-19; Rezaei, N., Ed.; Advances in Experimental Medicine and Biology; Springer: Cham, Swizerland, 2021; Volume 1318, pp. 705–725. [Google Scholar]
- Chen, Q.; Liang, M.; Li, Y.; Guo, J.; Fei, D.; Wang, L.; He, L.; Scheng, C.; Cai, Y.; Li, X.; et al. Mental health care for medical staff in China during the COVID-19 outbreak. Lancet Psychiatry 2020, 7, e15. [Google Scholar] [CrossRef] [PubMed]
- Freudenberger, H.J. Staff burn-out. J. Soc. Issues 1974, 30, 159–165. [Google Scholar] [CrossRef]
- Maslach, C. Burned-out. Can. J. Psychiatr. Nurs. 1979, 20, 5–9. [Google Scholar] [PubMed]
- Maslach, C. Burnout: The Cost of Caring; Prentice-Hall: Englewood Cliffs, NJ, USA, 1982. [Google Scholar]
- Leiter, M.; Maslach, C. Latent burnout profiles: A new approach to understanding the burnout experience. Burn. Res. 2016, 3, 89–100. [Google Scholar] [CrossRef]
- Uribe Prado, J.F. La Escala de Desgaste Ocupacional (EDO) y sus propiedades psicométricas con trabajadores en precariedad laboral de la Ciudad de México [The Occupational Burnout Scale (EDO) and its psychometric properties with precarious workers in Mexico City]. Rev. Interam. Psicol. Ocup. 2013, 32, 38–55. [Google Scholar]
- Maslach, C.; Leiter, M. Early predictors of job burnout and engagement. J. Appl. Psychol. 2008, 93, 498–512. [Google Scholar] [CrossRef]
- Drüge, M.; Schladitz, S.; Wirtz, M.A.; Schleider, K. Psychosocial burden and strains of pedagogues-using the Job Demands-Resources Theory to predict burnout, job satisfaction, general state of health, and life satisfaction. Int. J. Environ. Res. Public Health 2021, 18, 7921. [Google Scholar] [CrossRef]
- Kisely, S.; Warren, N.; McMahon, L.; Dalais, C.; Henry, I.; Siskind, D. Occurrence, prevention, and management of the psychological effects of emerging virus outbreaks on healthcare workers: Rapid review and meta-analysis. BMJ 2020, 369, m1642. [Google Scholar] [CrossRef]
- Rodriguez, R.M.; Medak, A.J.; Baumann, B.M.; Lim, S.; Chinnock, B.; Frazier, R.; Cooper, R.J. Academic emergency medicine physicians’ anxiety levels, stressors, and potential stress mitigation measures during the acceleration phase of the COVID-19 Pandemic. Acad. Emerg. Med. 2020, 27, 700–707. [Google Scholar] [CrossRef] [PubMed]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Andrade, G.; Menolli, P.; Clemente, P.; Eumann, A.; Silva, D.; Girotto, E. Burnout syndrome and consumption of alcohol and illicit substances in university students. Sch. Educ. Psychol. 2021, 31, e3134. [Google Scholar] [CrossRef]
- Bonini, A.D.; Campos, J.S.; Valéria Salloume Sampaio Bonafé, F.; Velez Oliveira, R.; Maroco, J. Burnout syndrome and alcohol consumption in prison employees. Rev. Bras. Epidemiol. 2016, 19, 205–216. [Google Scholar] [CrossRef]
- Jackson, E.R.; Shanafelt, T.D.; Hasan, O.; Satele, D.V.; Dyrbye, L.N. Burnout and alcohol abuse/dependence among U.S. medical students. Acad. Med. 2016, 91, 1251–1256. [Google Scholar] [CrossRef] [PubMed]
- Ahola, K.; Pulkki-Råback, L.; Kouvonen, A.; Rossi, H.; Aromaa, A.; Lönnqvist, J. Burnout and behavior-related health risk factors: Results from the population-based Finnish Health 2000 study. J. Occup. Environ. Med. 2012, 54, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Olivares-Faúndez, V.E.; Gil-Monte, P.R.; Figueiredo-Ferraz, H. The mediating role of feelings of guilt in the relationship between burnout and the consumption of tobacco and alcohol. Jpn. Psychol. Res. 2014, 56, 340–348. [Google Scholar] [CrossRef]
- Aaker, J.L. Dimensions of Brand Personality. J. Mark. Res. 1997, 34, 347–356. [Google Scholar] [CrossRef]
- Wiesner, M.; Windle, M.; Freeman, A. Work stress, substance use, and depression among young adult workers: An examination of main and moderator effect model. J. Occup. Health Psychol. 2005, 10, 83–96. [Google Scholar] [CrossRef]
- Frone, M.R. Are work stressors related to employee substance use? The importance of temporal context assessments of alcohol and illicit drug use. J. Appl. Psychol. 2008, 93, 199–206. [Google Scholar] [CrossRef]
- Beiter, K.J.; Wiedemann, R.P.; Thomas, C.L.; Conrad, E.J. Alcohol consumption and COVID-19–Related stress among health care workers: The need for continued stress-management mnterventions. Public Health Rep. 2022, 137, 326–335. [Google Scholar] [CrossRef]
- Medina-Mora, M.E.; Cordero-Oropeza, M.; Rafful, C.; Real, T.; Villatoro-Velazquez, J.A. COVID-19 and alcohol in Mexico: A serious health crisis, strong actions on alcohol in response—Commentary on Stockwell et al. Drug Alcohol Rev. 2021, 40, 13–16. [Google Scholar] [CrossRef]
- Raman, B.; Cassar, M.P.; Tunnicliffe, E.M.; Filippini, N.; Griffanti, L.; Alfaro-Almagro, F.; Okell, T.; Sheerin, F.; Xie, C.; Mahmod, M.; et al. Medium-term effects of SARS-CoV-2 infection on multiple vital organs, exercise capacity, cognition, quality of life and mental health, post-hospital discharge. EClinicalMedicine 2021, 31, 100683. [Google Scholar] [CrossRef]
- Nesoff, E.D.; Gutkind, S.; Sirota, S.; McKowen, A.L.; Veldhuis, C.B. Mental health and economic stressors associated with high-risk drinking and increased alcohol consumption early in the COVID-19 pandemic in the United States. Prev. Med. 2021, 153, 106854. [Google Scholar] [CrossRef] [PubMed]
- Pocuca, N.; London-Nadeau, K.; Geoffroy, M.-C.; Chadi, N.; Séguin, J.R.; Parent, S.; Boivin, M.; Tremblay, R.E.; Cote, S.M.; Costellanos-Ryan, N. Changes in emerging adults’ alcohol and cannabis use from before to during the COVID-19 pandemic: Evidence from a prospective birth cohort. Psychol. Addict. Behav. 2022, 36, 786–797. [Google Scholar] [CrossRef] [PubMed]
- Shield, K.D.; Chrystoja, B.R.; Ali, S.; Sohi, I.; Rehm, J.; Nigatu, Y.T.; Elton-Marshall, T.; Hamilton, H.; Jankowicz, D.; Wells, S. Changes in alcohol consumption in Canada during the COVID-19 Pandemic: Associations with anxiety and self-perception of depression and loneliness. Alcohol Alcohol. 2021, 57, 190–197. [Google Scholar] [CrossRef]
- Turaev Bobir, T. Patients with alcoholism functional changes in the liver after COVID-19 disease. Peerian J. 2023, 15, 38–47. [Google Scholar]
- Ji, D.; Qin, E.; Xu, J.; Zhang, D.; Cheng, G.; Wang, Y.; Lau, G. Non-alcoholic fatty liver diseases in patients with COVID-19: A retrospective study. J. Hepatol. 2020, 73, 451–453. [Google Scholar] [CrossRef]
- Xu, L.; Liu, J.; Lu, M.; Yang, D.; Zheng, X. Liver injury during highly pathogenic human coronavirus infections. Liver Int. 2020, 40, 998–1004. [Google Scholar] [CrossRef]
- Singh, A.; Hussain, S.; Antony, B. Non-alcoholic fatty liver disease and clinical outcomes in patients with COVID-19: A comprehensive systematic review and meta-analysis. Diabetes Metab. Syndr. Clin. Res. Rev. 2021, 15, 813–822. [Google Scholar] [CrossRef]
- Nielsen, M.B.; Finne, L.B.; Christensen, J.O.; Knardahl, S. Job demands and alcohol use: Testing a moderated mediation model. Scand. J. Work. Environ. Health 2015, 41, 43–53. [Google Scholar] [CrossRef]
- Bandura, A. Self-Efficacy: The Exercise of Control; W H Freeman/Times Books/Henry Holt & Co.: New York, NY, USA, 1997; Volume 9, p. 604. [Google Scholar]
- Bandura, A. Social Cognitive Theory: An agentic perspective. Annu. Rev. Psychol. 2001, 52, 21–41. [Google Scholar] [CrossRef]
- Makara-Studzińska, M.; Golonka, K.; Izydorczyk, B. Self-efficacy as a moderator between stress and professional burnout in firefighters. Int. J. Environ. Res. Public Health 2019, 16, 183. [Google Scholar] [CrossRef]
- Alessandri, G.; Perinelli, E.; De Longis, E.; Schaufeli, W.B.; Theodorou, A.; Borgogni, L.; Caprara, G.V.; Cinque, L. Job burnout: The contribution of emotional stability and emotional self-efficacy beliefs. J. Occup. Organ. Psychol. 2018, 91, 823–851. [Google Scholar] [CrossRef]
- Brown, C.G. A systematic review of the relationship between self-efficacy and burnout in teachers. Educ. Child Psychol. 2012, 29, 47–63. [Google Scholar] [CrossRef]
- Shoji, K.; Cieslak, R.; Smoktunowicz, E.; Rogala, A.; Benight, C.C.; Luszczynska, A. Associations between job burnout and self-efficacy: A meta-analysis. Anxiety Stress Coping 2016, 29, 367–386. [Google Scholar] [CrossRef] [PubMed]
- Maslach, C.; Jackson, S.E. The measurement of experienced burnout. J. Organ. Behav. 1981, 2, 99–113. [Google Scholar] [CrossRef]
- Franco-Díaz, K.L.; Fernández-Niño, J.A.; Astudillo-García, C.I. Prevalencia de síntomas depresivos e invarianza factorial de la Escala de Depresión del Centro de Estudios Epidemiológicos (CES-D) en población indígena mexicana [Prevalence of depressive symptoms and factorial invariance of the Center for Epidemiologic Studies (CES-D) Depression Scale in a group of Mexican indigenous population]. Biomédica 2018, 38, 127–140. [Google Scholar] [CrossRef] [PubMed]
- Herrero, J.; Gracia, E. Una medida breve de la sintomatología depresiva (CESD-7). Salud Ment. 2007, 30, 40–46. [Google Scholar]
- Balasubramanian, A.; Paleri, V.; Bennett, R.; Paleri, V. Impact of COVID-19 on the mental health of surgeons and coping strategies. Head Neck 2020, 42, 1638–1644. [Google Scholar] [CrossRef]
- Babor, T.F.; Higgins-Bidle, J.C.; Saunders, J.B.; Monteiro, M.G. Audit. Cuestionario de Identificación de los Trastornos Debidos al Consumo de Alcohol. Pautas para su Utilización en Atención Primaria [AUDIT. Questionnaire for the Identification of Disorders due to Alcohol Consumption. Guidelines for Its Use in Primary Care]; Sustancias, S.M., Ed.; Organización Mundial de la Salud/World Health Organization: Geneva, Switzerland, 2001. [Google Scholar]
- Harris, P.A.; Taylor, R.; Minor, B.L.; Elliott, V.; Fernandez, M.; O’Neal, L.; McLeod, L.; Delacqua, G.; Delacqua, F.; Kirby, J.; et al. The REDCap consortium: Building an international community of software platform partners. J. Biomed. Inform. 2019, 95, e103208. [Google Scholar] [CrossRef]
- IBM SPSS. AMOS. for Windows, 26.0.0 ed.; IBM Corporation: Wexford, PA, USA, 2019. [Google Scholar]
- IBM SPSS. For Windows, 26th ed.; IBM Corporation: Armonk, NY, USA, 2019. [Google Scholar]
- Cho, G.; Hwang, H.; Sarstedt, M.; Ringle, C.M. Cutoff criteria for overall model fit indexes in generalized structured component analysis. J. Mark. Anal. 2020, 8, 189–202. [Google Scholar] [CrossRef]
- Byrne, B.M. Structural equation modeling with AMOS, EQS, and LISREL: Comparative approaches to testing for the factorial validity of a measuring instrument. Int. J. Test. 2001, 1, 55–86. [Google Scholar] [CrossRef]
- Collier, J.E. Applied Structural Equation Modeling Using AMOS; Basic to Advanced Techniques; Routledge: New York, NY, USA, 2020. [Google Scholar]
- Mache, S.; Vitzthum, K.; Groneberg, D.A. Prevention of study-related stress symptoms: Health-promoting behavior among dental students. Wien. Med. Wochenschr. 2015, 165, 100–106. [Google Scholar] [CrossRef] [PubMed]
- Maslach, C.; Jackson, S.E.; Leiter, M. The Maslach Burnout Inventory-Test Manual, 3rd ed.; Consulting Psychologist Press: Palo Alto, CA, USA, 1996. [Google Scholar]
- Pietrowski, D.L.; Cardoso, N.D.O.; Bernardi, C.C.D.N. Estratégias de coping frente à síndrome de burnout entre os professores: Uma revisão integrativa da literatura nacional [Coping strategies for burnout syndrome between teachers: A national integrative literature review]. Contextos Clín. 2018, 11, 397–409. [Google Scholar] [CrossRef]
- Tsutsumi, A.; Kayaba, K.; Theorell, T.; Siegrist, J. Association between job stress and depression among Japanese employees threatened by job loss in a comparison between two complementary job-stress models. Scand. J. Work. Environ. Health 2001, 27, 146–153. [Google Scholar] [CrossRef] [PubMed]
- Airagnes, G.; Lemogne, C.; Even-Baisse, M.-A.; Le Faou, A.-L.; Limosin, F. Work conditions are associated with alcohol use after taking into account life conditions outside of work: Findings from a french occupational health service. Subst. Use Misuse 2021, 56, 2259–2263. [Google Scholar] [CrossRef]
- Hruska, B.; Barduhn, M.S. Dynamic psychosocial risk and protective factors associated with mental health in Emergency Medical Service (EMS) personnel. J. Affect. Disord. 2021, 282, 9–17. [Google Scholar] [CrossRef]
- Bardhoshi, G.; Um, B. The effects of job demands and resources on school counselor burnout: Self-efficacy as a mediator. J. Couns. Dev. 2021, 99, 289–301. [Google Scholar] [CrossRef]
- Kumar, N.; Gupta, M.; Gupta, D.; Tiwari, S. Novel deep transfer learning model for COVID-19 patient detection using X-ray chest images. J. Ambient. Intell. Humaniz. Comput. 2023, 14, 469–478. [Google Scholar] [CrossRef]
- Reis, H.C.; Turk, V. COVID-DSNet: A novel deep convolutional neural network for detection of coronavirus (SARS-CoV-2) cases from CT and Chest X-Ray images. Artif. Intell. Med. 2022, 134, 102427. [Google Scholar] [CrossRef]
- Calina, D.; Hartung, T.; Mardare, I.; Mitroi, M.; Poulas, K.; Tsatsakis, A.; Rogoveanu, I.; Docea, A.O. COVID-19 pandemic and alcohol consumption: Impacts and interconnections. Toxicol. Rep. 2021, 8, 529–535. [Google Scholar] [CrossRef]
- Valencia, P.D.; Torres-Quispe, M.A.; Sánchez-Cayo, S.; Reyes-Aguilar, R.F.; Acevedo-Cahuana, A.G. Factors associated with depressive symptomatology during the COVID-19 pandemic in Mexico: A 2021 national survey. J. Affect. Disord. 2022, 317, 212–220. [Google Scholar] [CrossRef]
Figure 1.
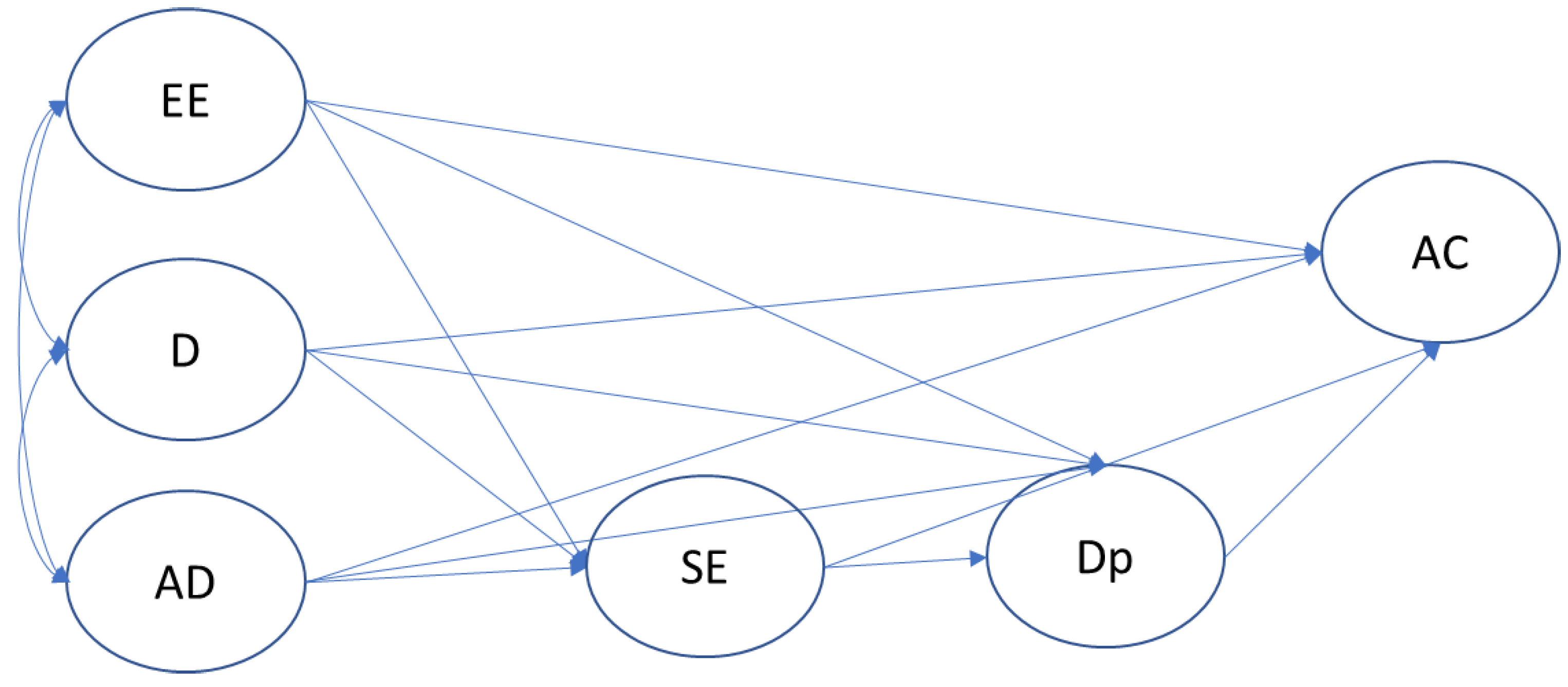
Mediation model of self-efficacy and depression between burnout and alcohol consumption. Latent constructs are shown in circles, and observable variables and error terms are not shown; double-headed arrows represent covariances, and single arrows represent direct effects. EE = Emotional Exhaustion; D = Depersonalization; AD = Achievement Dissatisfaction; SE = Self-Efficacy; Dp = Depression; AC = Alcohol Consumption.
Figure 1.
Mediation model of self-efficacy and depression between burnout and alcohol consumption. Latent constructs are shown in circles, and observable variables and error terms are not shown; double-headed arrows represent covariances, and single arrows represent direct effects. EE = Emotional Exhaustion; D = Depersonalization; AD = Achievement Dissatisfaction; SE = Self-Efficacy; Dp = Depression; AC = Alcohol Consumption.
Table 1.
Structural equation model of burnout predicting alcohol consumption.
Table 1.
Structural equation model of burnout predicting alcohol consumption.
| Relationships | B | S.E. | C.R. | β | p |
|---|---|---|---|---|---|
| Emotional Exhaustion → | |||||
| Self-Efficacy at Work | −0.20 | 0.03 | −7.07 | −0.18 | <0.001 |
| Depression | 0.60 | 0.03 | 24.59 | 0.54 | <0.001 |
| Alcohol Consumption | −0.02 | 0.02 | −1.08 | −0.04 | 0.279 |
| Depersonalization → | |||||
| Self-Efficacy at Work | −0.21 | 0.03 | −6.25 | −0.15 | <0.001 |
| Depression | 0.14 | 0.03 | 5.33 | 0.10 | <0.001 |
| Alcohol Consumption | 0.10 | 0.02 | 5.89 | 0.15 | <0.001 |
| Achievement Dissatisfaction → | |||||
| Self-Efficacy at Work | −0.19 | 0.04 | −4.86 | −0.12 | <0.001 |
| Depression | 0.18 | 0.03 | 5.79 | 0.12 | <0.001 |
| Alcohol Consumption | 0.00 | 0.02 | 0.21 | 0.01 | 0.835 |
| Self-Efficacy at Work → | |||||
| Depression | −0.11 | 0.02 | −7.53 | −0.11 | <0.001 |
| Alcohol Consumption | −0.02 | 0.01 | −2.19 | −0.04 | 0.029 |
| Depression → | |||||
| Alcohol Consumption | 0.08 | 0.01 | 6.19 | 0.18 | <0.001 |
Table 2.
Indirect effects of burnout and self-efficacy on alcohol consumption.
Table 2.
Indirect effects of burnout and self-efficacy on alcohol consumption.
| B | Confidence Interval | p | ||
|---|---|---|---|---|
| Low | High | |||
| EE -> D -> AC | 0.049 | 0.035 | 0.066 | 0.006 |
| EE -> SE -> AC | 0.004 | 0.001 | 0.007 | 0.030 |
| EE -> SE -> D -> AC | 0.002 | 0.001 | 0.003 | 0.004 |
| DEP -> D -> AC | 0.011 | 0.007 | 0.017 | 0.012 |
| DEP -> SE -> AC | 0.004 | 0.002 | 0.009 | 0.014 |
| DEP -> SE -> D -> AC | 0.002 | 0.001 | 0.003 | 0.004 |
| AD -> D -> AC | 0.014 | 0.009 | 0.020 | 0.008 |
| AD -> SE ->AC | 0.004 | 0.001 | 0.009 | 0.013 |
| AD -> SE -> D -> AC | 0.002 | 0.001 | 0.003 | 0.002 |
| SE-> D ->AC | −0.009 | −0.013 | −0.006 | 0.004 |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
[ad_2]