COVID | Free Full-Text | Peritraumatic Distress among Chinese Canadians during the Early Lockdown Stage of the COVID-19 Pandemic: Sociodemographic and Pandemic-Related Predictors
[ad_1]
1. Introduction
1.1. The Psychological Impact of the Pandemic
1.2. Chinese Canadian Population
1.3. Sociodemographic Variables
1.4. Pandemic-Related Variables
1.5. Coping and Life Satisfaction
1.6. Present Study
2. Materials and Methods
2.1. Participants
2.2. Materials
2.2.1. The COVID-19 Peritraumatic Distress Index (CPDI)
2.2.2. Sociodemographic Variables
Sociodemographic information was collected, including age, gender, education level, marital status, employment status, citizenship status, place of birth, how long they have been in Canada, the number of people living in the same residence (i.e., housing size), income level (scaled from 1 to 5), and self-rated physical, mental, and sleep health.
2.2.3. Pandemic-related Variables (Experiences, Cognitions, and Behaviours)
The survey also includes questions on COVID-19-related experiences, cognition, and behaviours. For COVID-19 experiences, the four items assessing diagnosis/exposure status of the self and others who are close (e.g., “have you been diagnosed with the COVID-19?” for self diagnosis status and “are there any confirmed or suspected COVID-19 cases among your friends, family, or colleagues?” for other diagnosis statuses) were merged into one index for the infection/exposure status (“Yes” or “No/missing”). Another COVID-19 experience item assessed the action experiences related to COVID-19 (“did you have any of the following experiences during the pandemic”, with options such as self-isolation, fundraising, volunteering, donations, etc.).
COVID-19 cognitions were assessed with 10 items as follows: (1) infection likeliness (“how likely you will be infected with COVID?”); (2) self/family contraction worry (e.g., “are you afraid that yourself/family contracting the virus?”); (3) COVID-19 information authenticity (e.g., “are you bothered by the authenticity of the information received on COVID pandemic”); (4) Canada measure attitude (“your attitudes towards Canada’s measure?”); (5) threat perception (e.g., “do you believe the COVID-19 pandemic is a real threat?)”; (6) discrimination perception (e.g., “do you think that the COVID-19 breakout will result in prejudice and discrimination against Chinese in Canada?”); (7) 4 items on future infection predictions (e.g., “estimate the percentage of the population in your community/Ontario /Canada/World that will be infected by the COVID-19.”); (8) 6 items on personal measure effectiveness perception (e.g., “how effective do you think the following measures in restricting the spread of the virus”); and (9) 5 items on the level of public measure support (e.g., “to which degree do you support the following COVID-restriction public measures?”). Nearly all these items employed a 5-point Likert scale ranging from 1 (“strongly agree”) to 5 (“strongly disagree”), except for the outbreak threat perception items that used a text-entry format. All these variables were thus analyzed as continuous variables.
COVID-19 behaviours were assessed in a dichotomized format (i.e., “Yes” or “No/missing”) for the engagement of nine different behavioural preventative measures in the past week (e.g., “avoided crowded places?”, “cleaning/disinfecting rooms”, or “stocking food and good?”).
2.2.4. Moderator Variables
At the end of the survey, coping behaviour endorsement was further addressed through two multiple-choice questions. The first question (“Which of the following methods do you usually use to reduce stress/anxiety?”) identifies commonly used stress coping behaviours by responding (“Yes” or “No”) to a list of potential behaviours (i.e., exercise, listening to music, reading, drinking tea, and/or chatting with friends/family). The second question (“What kind of music can effectively help you relieve your emotions?”) identifies (“Yes” or “No”) the genre of music (i.e., classical, nature sound, pop, religious, love) that was perceived as being effective in mood regulation. Each of these options were coded as a dichotomous variable (“Yes” or “No”).
The Satisfaction with Life Scale (SWLS; Pavot and Diener, 1993) assesses the global perception of life satisfaction with 5 items based on a 7-point Likert scale from 1 (strongly disagree) to 7 (strongly agree). The sum score (ranged 5–35) was used to index life satisfaction, with a higher score meaning higher satisfaction. The SWLS has a strong internal reliability (as = 0.79–0.89) and moderate temporal stability (rs = 0.50–0.84 over 2 weeks to 4 years) (Pavot and Diener, 1993). The current sample in this study also showed a strong internal reliability (a = 0.94).
2.3. Statistical Analysis Approach
Data were analyzed in IBM SPSS Statistics for Windows, Version 23 (IBM Corp., Armonk, NY, USA). Given the high number of independent variables, in order to ensure statistical power, we separately analyzed sociodemographic variables and COVID-19-related variables (i.e., behaviours, cognitions, and experiences) as predictors in two regression models for the outcome variable (i.e., the CPDI score). To best capture the variance in the CPDI and for clarity consideration, some predictive variables were simplified by being recoded into binary or either 3-level or 4-level categorical variables based on the preliminary frequency analysis on the CPDI score distribution across the options of each predictive variable. For example, age was coded into three levels (i.e., 18 to 34, 35 to 64, and 65 or older) and gender was coded into female and male. Based on a principal component factor analysis of the three 5-point items for health status (mental health, physical health, and sleep quality), a single-factor (λ = 2.18) was extracted (λ = 2.23, loading = 0.82–0.90), which was indexed by a composite score for general health status. Multiple factor analyses were conducted for the COVID-19 experience, cognition, and behaviour items. One factor was extracted from the four future infection prediction items (λ = 3.36, loading = 0.86–0.96). Two factors were extracted from the six items on personal measure perception as follows: behavioural measures (4 items on hand-washing, mask-wearing, disinfection, and reducing going out, respectively; λ = 3.21, loading = 0.76–0.84) and health hygiene (2 items on salt water gargling and taking vitamin C or other health products, respectively; λ = 1.17, loading = 0.91–0.93). One factor was extracted from the five items on public measure support (λ = 2.71, loading = 0.30–0.86). Finally, two factors were extracted from the nine behavioural preventative measure engagement items as follows: avoidance behaviours (e.g., “avoid eating out”, “avoid public transportation”, “avoid crowding public places”, “avoiding visiting relatives and friends”, and “cancelling travel plans”; λ = 2.78, loading = 0.58–0.74) and endorsement behaviours (e.g., “stocking food and grocery items”, “cleaning/disinfecting rooms”, “maintaining indoor air circulation”, and “personal hygiene practices such as hand-washing and mask-wearing”; λ = 1.43, loading = 0.45–0.78).
3. Results
3.1. Sample Characteristics
3.2. Sociodemographic Predictors for the CPDI
3.3. Pandemic-Related Predictors of the CPDI
Table 5.
Linear regression of the Pandemic-related predictors of the CPDI (N = 378).
Table 5.
Linear regression of the Pandemic-related predictors of the CPDI (N = 378).
| Step | Predictors | CPDI | ||||
|---|---|---|---|---|---|---|
| β | 95% CI | R2 | F | |||
| 1 | SWLS | −1.20 *** | −1.40, −0.99 | 0.29 | 27.44 *** | |
| Coping: Exercise | Yes (reference) No/missing |
1.00 | −1.53, 3.53 | |||
| Coping: Reading | Yes (reference) No/missing |
0.32 | −2.12, 2.77 | |||
| Coping: Pop music | Yes (reference) No/missing |
2.18 | −0.34, 4.70 | |||
| Coping: Love song | Yes (reference) No/missing |
1.13 | −1.78, 4.04 | |||
| 2 | SWLS | −1.02 *** | −1.21, −0.82 | 0.43 | 17.52 *** | |
| Coping: Exercise | Yes (reference) No/missing |
0.18 | −2.08, 2.45 | |||
| Coping: Reading | Yes (reference) No/missing |
0.49 | −1.69, 2.66 | |||
| Coping: Pop music | Yes (reference) No/missing |
2.23 | −0.01, 4.48 | |||
| Coping: Love song | Yes (reference) No/missing |
0.48 | −2.12, 3.07 | |||
| COVID-19 experience: Infection/exposure |
Yes (reference) | |||||
| No/missing | 0.64 | −2.96, 4.25 | ||||
| Action | Yes (reference) | |||||
| No/missing | 2.32 | −0.74, 5.38 | ||||
| COVID-19 behaviour: Avoidance |
Yes (reference) | |||||
| No/missing | 4.33 | −7.80, 16.46 | ||||
| COVID-19 cognition: Infection likeliness |
1 = lowest, 5 = highest | −0.76 | −2.12, 0.61 | |||
| Self-contraction worry | 1 = lowest, 5 = highest | 3.38 *** | 1.73, 5.04 | |||
| Family-contraction worry | 1 = lowest, 5 = highest | 0.33 | −1.28, 1.93 | |||
| Information authenticity concern | 1 = lowest, 5 = highest | 2.16 *** | 0.99, 3.34 | |||
| Canada measure attitude | 1 = very positive, 5 = very negative |
−0.60 | −1.56, 0.36 | |||
| Threat perception | 1 = lowest, 5 = highest | 1.07 | −0.40, 2.55 | |||
| Discrimination perception | 1 = lowest, 5 = highest | 0.92 | −0.28, 2.11 | |||
| Future infection prediction | 0–100% | 0.10 ** | 0.04, 0.17 | |||
| Personal health hygiene | 1 = completely ineffective, 5 = completely effective |
1.61 ** | 0.46, 2.76 | |||
4. Discussion
The purpose of this study was to identify sociodemographic and pandemic-related variables (i.e., experiences, perceptions, and/or behaviours) that may be predictors of psychological distress among Chinese residents living in Canada during the first lockdown period of the pandemic (April–May, 2020). Overall, this study identified several sociodemographic risk factors including being in the middle-aged group (aged 35–64) relative to young adults, living in Ontario (relative to elsewhere), and a poor health status, as well as a few COVID-19-related cognition risk factors (i.e., self-contraction worry, COVID-19 information authenticity concern, future infection rate prediction, and personal health hygiene effectiveness rating). Additionally, certain variables were found to buffer distress in this population, including being retired or a student (relative to being employed) and/or higher life satisfaction.
4.1. Sociodemographic Predictors
4.2. Pandemic-Related Predictors
4.3. Perceived Racial Discrimination
5. Limitations
In the context of the elevated proportion of highly educated, middle-aged (aged 35 to 64 years), employed, and female respondents, convenience sampling may have restricted the generalizability of the findings as certain social groups (e.g., unemployed, low education) were underrepresented in the sample. Furthermore, the coping behaviour endorsement variables were all responded to through a dichotomous Yes/No, which may have restricted the variance of these variables and thus masked their prediction of psychological distress. However, it should be noted that the low frequencies of these behaviours likely match natural variation in the population given the stringent COVID-19 precautions during this period. Given the known relationship between acculturation and psychological well-being, the influence of acculturation over COVID-19-related psychological distress was not assessed, thus representing a potential future avenue of research.
6. Conclusions and Implications
In conclusion, the present research identifies life satisfaction as a consistent buffering predictor of distress experienced at the early stage of the pandemic. Additionally, by controlling for life satisfaction, the results identified a number of sociodemographic risk factors for experiencing psychological distress, including being middle-aged, employed (relative to retired people/students), living in Ontario (rather than elsewhere), and a poor health status. Additionally, this study identified a number of pandemic-related risk factors for distress, including a higher self-contraction worry, more of a COVID-19 information authenticity concern, a higher future infection rate prediction, and a higher personal health hygiene appraisal.
These findings add to the existing literature by identifying relevant COVID-19-related predictors and specifically focusing on Chinese immigrant populations. Moreover, the study contributes meaningful cognitive and behavioural data at the earliest onset of a pandemic. As such, these findings offer significant insights that can inform more focused strategies for prevention and intervention practices, with the intention of alleviating stress and mental health repercussions in a minoritized population and better preparing them for future possible public health crises like a pandemic. For examples, in light of the findings from the current study, future practice and policies related to post-pandemic mental health prevention/intervention among minoritized population should target those in the middle-age (35–64 year old), employed (relative to retired people/students), or in poor health condition sub-groups because they are particularly vulnerable to COVID-related distress. Additionally, resources and practices should be directed to reduce the self-contraction worry, enhance information authenticity, mitigate risk prediction (e.g., infection rate), and increase awareness/knowledge of personal health hygiene because these factors are likely related to general psychological distress during the pandemic.
Author Contributions
Conceptualization, L.Y.; methodology, L.Y., K.K. and A.K.; validation, K.K.; formal analysis, K.K., A.K. and L.Y.; resources, A.K., K.K. and L.Y.; data curation, L.Y.; writing—original draft, A.K. and K.K; writing—review and editing, A.K., K.K. and L.Y.; visualization, K.K., A.K. and L.Y.; supervision, K.K. and L.Y.; project administration, L.Y.; funding acquisition, L.Y. All authors have read and agreed to the published version of the manuscript.
Funding
This work was funded by the New Frontiers Research Fund through the Canadian Institute of Health Research (CIHR) [NFRF-2019-00012] awarded to Lixia Yang (with Dr. Peizhong Wang).
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Ryerson University [REB 2020-132] and Memorial University of Newfoundland [20201772-ME].
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
Acknowledgments
We would like to thank Helen Cao for their diligent support in participant recruitment and data collection. We also thank Peizhong Wang, Weiguo Zhang, and Xiaolin Wei for their contribution to their guidance during the survey building at the early stage of this project.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- World Health Organization. 10 Global Health Issues to Track in 2021; World Health Organization: Geneva, Switzerland, 2020; Available online: https://www.who.int/news-room/spotlight/10-global-health-issues-to-track-in-2021 (accessed on 30 April 2021).
- Nwachukwu, I.; Nkire, N.; Shalaby, R.; Hrabok, M.; Vuong, W.; Gusnowski, A.; Surood, S.; Urichuk, L.; Greenshaw, A.J.; Agyapong, V.I. COVID-19 Pandemic: Age-related differences in measures of stress, anxiety and depression in Canada. Int. J. Environ. Res. Public Health 2020, 17, 6366. [Google Scholar] [CrossRef]
- Kowal, M.; Coll-Martín, T.; Ikizer, G.; Rasmussen, J.; Eichel, K.; Studzińska, A.; Koszałkowska, K.; Karwowski, M.; Najmussaqib, A.; Pankowski, D.; et al. Who is the Most Stressed During the COVID-19 Pandemic? Data From 26 Countries and Areas. Appl. Psychol. Health Wellbeing 2020, 12, 946–966. [Google Scholar] [CrossRef]
- Banerjee, D.; Vaishnav, M.; Rao, T.S.; Raju, V.K.; Dalal, P.; Javed, A.; Saha, G.; Mishra, K.K.; Kumar, V.; Jagiwala, M.P. Impact of the COVID-19 pandemic on psychosocial health and well-being in South-Asian (World Psychiatric Association zone 16) countries: A systematic and advocacy review from the Indian Psychiatric Society. Indian J. Psychiatry 2020, 62, 343. [Google Scholar] [CrossRef] [PubMed]
- Shah, S.M.A.; Mohammad, D.; Qureshi, M.F.H.; Abbas, M.Z.; Aleem, S. Prevalence, Psychological Responses and Associated Correlates of Depression, Anxiety and Stress in a Global Population, during the Coronavirus Disease (COVID-19) Pandemic. Community Ment. Health J. 2021, 57, 101–110. [Google Scholar] [CrossRef] [PubMed]
- Haft, S.L.; Zhou, Q. An Outbreak of Xenophobia: Perceived discrimination and anxiety in Chinese American college students before and during the COVID-19 pandemic. Int. J. Psychol. 2021, 56, 522–531. [Google Scholar] [CrossRef]
- Sorokowski, P.; Groyecka, A.; Kowal, M.; Sorokowska, A.; Białek, M.; Lebuda, I.; Dobrowolska, M.; Zdybek, P.; Karwowski, M. Can Information about Pandemics Increase Negative Attitudes Toward Foreign Groups?: A case of COVID-19 outbreak. Sustainability 2020, 12, 4912. [Google Scholar] [CrossRef]
- Wang, Y.; Kala, M.P.; Jafar, T.H. Factors associated with psychological distress during the coronavirus disease 2019 (COVID-19) pandemic on the predominantly general population: A systematic review and meta-analysis. PLoS ONE 2020, 15, e0244630. [Google Scholar] [CrossRef]
- Watson, M.F.; Bacigalupe, G.; Daneshpour, M.; Han, W.; Parra-Cardona, R. COVID-19 Interconnectedness: Health inequity, the climate crisis, and collective trauma. Fam. Process. 2020, 59, 832–846. [Google Scholar] [CrossRef]
- Yang, L.; Kandasamy, K.; Na, L.; Zhang, W.; Wang, P.P. Perceived and experienced anti-Chinese discrimination and its associated psychological impacts among Chinese Canadians during the Wave 2 of the COVID-19 pandemic. Psychol. Health Med. 2022, 29, 108–125. [Google Scholar] [CrossRef]
- Fawaz, M.; Samaha, A. COVID-19 Quarantine: Post-traumatic stress symptomatology among Lebanese citizens. Int. J. Soc. Psychiatry 2020, 66, 666–674. [Google Scholar] [CrossRef]
- Landi, G.; Pakenham, K.I.; Boccolini, G.; Grandi, S.; Tossani, E. Health Anxiety and Mental Health Outcome during COVID-19 Lockdown in Italy: The mediating and moderating roles of psychological flexibility. Front. Psychol. 2020, 11, 2195. [Google Scholar] [CrossRef]
- Ramírez, L.P.; Arriaga, R.J.; Hernández-Gonzalez, M.; Roca-Chiapas, J.M. Psychological Distress and Signs of Post-Traumatic Stress in Response to the COVID-19 Health Emergency in a Mexican Sample. Psychol. Res. Behav. Manag. 2020, 13, 589–597. [Google Scholar] [CrossRef]
- Traunmüller, C.; Stefitz, R.; Gaisbachgrabner, K.; Schwerdtfeger, A. Psychological Correlates of COVID-19 Pandemic in the Austrian Population. BMC Public Health 2020, 20, 1395. [Google Scholar] [CrossRef]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; McIntyre, R.S.; Choo, F.N.; Tran, B.; Ho, R.; Sharma, V.K.; et al. A Longitudinal Study on the Mental Health of General Population during the COVID-19 Epidemic in China. Brain Behav. Immun. 2020, 87, 40–48. [Google Scholar] [CrossRef]
- Filindassi, V.; Pedrini, C.; Sabadini, C.; Duradoni, M.; Guazzini, A. Impact of COVID-19 First Wave on Psychological and Psychosocial Dimensions: A Systematic Review. COVID 2022, 2, 273–340. [Google Scholar] [CrossRef]
- Thomson, M.S.; Chaze, F.; George, U.; Gurgue, S. Improving Immigrant Populations’ Access to Mental Health Services in Canada: A Review of Barriers and Recommendations. J. Immigr. Minor. Health 2015, 17, 1895–1905. [Google Scholar] [CrossRef] [PubMed]
- Yu, S.; Kowitt, S.D.; Fisher, E.B.; Li, G. Mental Health in China: Stigma, family obligations, and the potential of peer support. Community Ment. Health J. 2017, 54, 757–764. [Google Scholar] [CrossRef]
- Heidinger, L.; Cotter, A. Perceptions of Personal Safety Among Population Groups Designated as Visible Minorities in Canada during the COVID-19 Pandemic. 2020. Available online: https://www150.statcan.gc.ca/n1/pub/45-28-0001/2020001/article/00046-eng.htm (accessed on 30 April 2021).
- The Social and Economic Impacts of COVID-19: A Six-Month Update—ARCHIVED. (n.d.). Available online: https://www150.statcan.gc.ca/n1/pub/11-631-x/11-631-x2020004-eng.pdf (accessed on 22 February 2021).
- Lecompte, M.; Counsell, A.; Yang, L. Demographic and COVID experience predictors of COVID-19 risk perception among Chinese residents in Canada. Int. J. Environ. Res. Public Health 2022, 19, 14448. [Google Scholar] [CrossRef] [PubMed]
- Lee, A.D.Y.; Wang, P.P.; Zhang, W.; Yang, L. COVID-19 Peritraumatic Distress and Loneliness in Chinese Residents in North America: The Role of Contraction Worry. Int. J. Environ. Res. Public Health 2022, 19, 7639. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Yu, L.; Kandasamy, K.; Wang, Y.; Shi, F.; Zhang, W.; Wang, P.P. Non-pathological psychological distress among Mainland Chinese in Canada and its sociodemographic risk factors amidst the pandemic. HealthCare 2022, 10, 2326. [Google Scholar] [CrossRef] [PubMed]
- Yu, L.; Lecompte, M.; Zhang, W.; Wang, P.; Yang, L. Sociodemographic and COVID-Related Predictors for Mental Health Condition of Mainland Chinese in Canada Amidst the Pandemic. Int. J. Environ. Res. Public Health 2022, 19, 171. [Google Scholar] [CrossRef]
- Forte, G.; Favieri, F.; Tambelli, R.; Casagrande, M. COVID-19 Pandemic in the Italian Population: Validation of a post-traumatic stress disorder questionnaire and prevalence of PTSD symptomatology. Int. J. Environ. Res. Public Health 2020, 17, 4151. [Google Scholar] [CrossRef]
- Carpenter, T.; Grecian, S.M.; Reynolds, R.M. Sex differences in early-life programming of the hypothalamic–pituitary–adrenal axis in humans suggest increased vulnerability in females: A systematic review. J. Dev. Orig. Health Dis. 2017, 8, 244–255. [Google Scholar] [CrossRef] [PubMed]
- Catuzzi, J.E.; Kevin, D.B. Anxiety Vulnerability in Women: A two-hit hypothesis. Exp. Neurol. 2014, 259, 75–80. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.-K. Analyzing the Gender Division of Labor: The Cases of the United States and South Korea. Asian Perspect. 2009, 33, 181–229. [Google Scholar] [CrossRef]
- Na, L.; Yang, L.; Mezo, P.G.; Liu, R. Age disparities in mental health during the COVID19 pandemic: The roles of resilience and coping. Soc. Sci. Med. 2022, 305, 115031. [Google Scholar] [CrossRef] [PubMed]
- Gao, J.; Zheng, P.; Jia, Y.; Chen, H.; Mao, Y.; Chen, S.; Wang, Y.; Fu, H.; Dai, J. Mental health problems and social media exposure during COVID-19 outbreak. PLoS ONE 2020, 15, e0231924. [Google Scholar]
- Qiu, J.; Shen, B.; Zhao, M.; Wang, Z.; Xie, B.; Xu, Y. A Nationwide Survey of Psychological Distress Among Chinese People in the COVID-19 Epidemic: Implications and policy recommendations. Gen. Psychiatry 2020, 33, e100213. [Google Scholar] [CrossRef] [PubMed]
- Limcaco, R.S.G.; Mateos, M.E.; Fernandez, M.J.; Roncero, C. Anxiety, Worry, and Perceived Stress in the World Due to the COVID-19 Pandemic. medRxiv 2020. [Google Scholar] [CrossRef]
- Farquharson, W.H.; Thornton, C.J. Debate: Exposing the most serious infirmity–Racism’s impact on health in the era of COVID-19. Child. Adolesc. Ment. Health 2020, 25, 182–183. [Google Scholar] [CrossRef]
- Rudenstine, S.; McNeal, K.; Schulder, T.; Ettman, C.K.; Hernandez, M.; Gvozdieva, K.; Galea, S. Depression and Anxiety during the COVID-19 Pandemicc in an Urba, Low-Income Public University Sample. J. Trauma. Stress 2021, 34, 12–22. [Google Scholar] [CrossRef] [PubMed]
- Daly, Z.; Slemon, A.; Richardson, C.G.; Salway, T.; McAuliffe, C.; Gadermann, A.M.; Thomson, K.C.; Hirani, S.; Jenkins, E.K. Associations between periods of COVID-19 quarantine and mental health in Canada. Psychiatry Res. 2021, 295, 113631. [Google Scholar] [CrossRef] [PubMed]
- Leung, G.M.; Lam, T.H.; Ho, L.M.; Ho, S.Y.; Chan, B.H.; Wong, I.O.; Hedley, A.J. The Impact of Community Psychological Responses on Outbreak Control for Severe Acute Respiratory Syndrome in Hong Kong. J. Epidemiol. Community Health 2003, 57, 857–863. [Google Scholar] [CrossRef]
- Dong, L.; Katsiris, A.; Lecompte, M.; Skrotzki, C.; Yang, L. A Qualitative Analysis of Older Adults’ Cognitive Appraisal in Coping during the COVID-19 Pandemic: The Role of Social Capital. COVID 2023, 3, 1622–1638. [Google Scholar] [CrossRef]
- Eichelberger, L. SARS and New York’s Chinatown: The politics of risk and blame during an epidemic of fear. Soc. Sci. Med. 2007, 65, 1284–1295. [Google Scholar] [CrossRef]
- Kong, J.; Ip, J.; Huang, C.; Lin, K.; Lin, F.; Yuen, C. A Year of Racist Attacks: Anti-Asian Racism across Canada One Year into the COVID-19 Pandemic. 2020. Available online: https://immigrantcovid.umn.edu/anti-asian-xenophobia (accessed on 30 April 2021).
- Carver, C.S. You want to measure coping but your protocol’s too long: Consider the brief COPE. Int. J. Behav. Med. 1997, 4, 92–100. [Google Scholar] [CrossRef]
- Vagni, M.; Maiorano, T.; Giostra, V.; Pajardi, D. Coping With COVID-19: Emergency Stress, Secondary Trauma and Self-Efficacy in Healthcare and Emergency Workers in Italy. Front. Psychol. 2020, 11, 566912. [Google Scholar] [CrossRef] [PubMed]
- Vagni, M.; Maiorano, T.; Giostra, V.; Pajardi, D.; Bartone, P. Emergency Stress, Hardiness, Coping Strategies and Burnout in Health Care and Emergency Response Workers during the COVID-19 Pandemic. Front. Psychol. 2022, 13, 918788. [Google Scholar] [CrossRef]
- Xiao, H.; Zhang, Y.; Kong, D.; Li, S.; Yang, N. The Effects of Social Support on Sleep Quality of Medical Staff Treating Patients with Coronavirus Disease 2019 (COVID-19) in January and February 2020 in China. Med. Sci. Monit. Int. Med. J. Exp. Clin. Res. 2020, 26, e923549. [Google Scholar] [CrossRef]
- Badon, S.E.; Croen, L.A.; Ferrara, A.; Ames, J.L.; Hedderson, M.M.; Young-Wolff, K.C.; Zhu, Y.; Avalos, L.A. Coping strategies for COVID-19 pandemic-related stress and mental health during pregnancy. J. Affect. Disord. 2022, 309, 309–313. [Google Scholar] [CrossRef]
- Diener, E.; Emmons, R.A.; Larsen, R.J.; Griffin, S. The satisfaction with life scale. J. Personal. Assess. 1985, 49, 71–75. [Google Scholar] [CrossRef]
- Dymecka, J.; Gerymski, R.; Machnik-Czerwik, A.; Derbis, R.; Bidzan, M. Fear of COVID-19 and Life Satisfaction: The Role of the Health-Related Hardiness and Sense of Coherence. Front. Psychiatry 2021, 12, 712103. [Google Scholar] [CrossRef]
- Martins, V.; Serrão, C.; Teixeira, A.; Castro, L.; Duarte, I. The mediating role of life satisfaction in the relationship between depression, anxiety, stress and burnout among Portuguese nurses during COVID-19 pandemic. BMC Nurs. 2022, 21, 188. [Google Scholar] [CrossRef] [PubMed]
- Padmanabhanunni, A.; Pretorius, T.B.; Isaacs, S.A. Satisfied with Life? The Protective Function of Life Satisfaction in the Relationship between Perceived Stress and Negative Mental Health Outcomes. Int. J. Environ. Res. Public Health 2023, 20, 6777. [Google Scholar] [CrossRef] [PubMed]
- Breslau, J.; Finucane, M.L.; Locker, A.R.; Baird, M.D.; Roth, E.A.; Collins, R.L. A longitudinal study of psychological distress in the United States before and during the COVID-19 pandemic. Prev. Med. 2021, 143, 106362. [Google Scholar] [CrossRef] [PubMed]
- Thomala, L.L. China: Most Popular Social Media Platforms 2019. 2020. Available online: https://www.statista.com/statistics/250546/leading-social-network-sites-in-china/ (accessed on 13 December 2020).
- Qian, M.; Wu, Q.; Wu, P.; Hou, Z.; Liang, Y.; Cowling, B.J.; Yu, H. Psychological responses, behavioral changes and public perceptions during the early phase of the COVID-190 outbreak in China: A population based cross-sectional survey. medRxiv 2020. [Google Scholar] [CrossRef]
- Chandu, V.C.; Marella, Y.; Panga, G.S.; Pachava, S.; Vadapalli, V. Measuring the Impact of COVID-19 on Mental Health: A scoping review of the existing scales. Indian J. Psychol. Med. 2020, 42, 421–427. [Google Scholar] [CrossRef]
- Steyerberg, E.W. Clinical Prediction Models A Practical Approach to Development, Validation, and Updating; Springer International Publishing: Cham, Switzerland, 2019; ISBN 3-030-16399-7. [Google Scholar]
- Einav, M.; Margalit, M. Loneliness before and after COVID-19: Sense of Coherence and Hope as Coping Mechanisms. Int. J. Environ. Res. Public Health 2023, 20, 5840. [Google Scholar] [CrossRef]
- Vlake, J.H.; Wesselius, S.; van Genderen, M.E.; van Bommel, J.; Boxma-de Klerk, B.; Wils, E.J. Psychological distress and health-related quality of life in patients after hospitalization during the COVID-19 pandemic: A single-center, observational study. PLoS ONE 2021, 16, e0255774. [Google Scholar] [CrossRef]
- Lewis, B.A.; Billing, L.; Schuver, K.; Gjerdingen, D.; Avery, M.; Marcus, B.H. The relationship between employment status and depression symptomatology among women at risk for postpartum depression. Women’s Health 2017, 13, 3–9. [Google Scholar] [CrossRef]
- Breslau, J.; Roth, E.A.; Baird, M.D.; Carman, K.G.; Collins, R.L. A longitudinal study of predictors of serious psychological distress during COVID-19 pandemic. Psychol. Med. 2023, 53, 2418–2426. [Google Scholar] [CrossRef] [PubMed]
- Zaccari, V.; D’Arienzo, M.C.; Caiazzo, T.; Magno, A.; Amico, G.; Mancini, F. Narrative review of COVID-19 impact on obsessive-compulsive disorder in child, adolescent and adult clinical populations. Front. Psychiatry 2021, 12, 673161. [Google Scholar] [CrossRef] [PubMed]
- Audet, J.S.; Jacmin-Park, S.; Kheloui, S.; Gravel, C.; Juster, R.P.; Aardema, F. COVID-19 related stress and fears of contamination: The impact of feared self-perceptions. Curr. Psychol. 2023; advance online publication. [Google Scholar] [CrossRef] [PubMed]
- Paredes, M.R.; Apaolaza, V.; Fernandez-Robin, C.; Hartmann, P.; Yañez-Martinez, D. The impact of the COVID-19 pandemic on subjective mental well-being: The interplay of perceived threat, future anxiety and resilience. Personal. Individ. Differ. 2021, 170, 110455. [Google Scholar] [CrossRef]
- Yue, Z.; Zhang, R.; Xiao, J. Passive social media use and psychological well-being during the COVID-19 pandemic: The role of social comparison and emotion regulation. Comput. Hum. Behav. 2022, 127, 107050. [Google Scholar] [CrossRef]
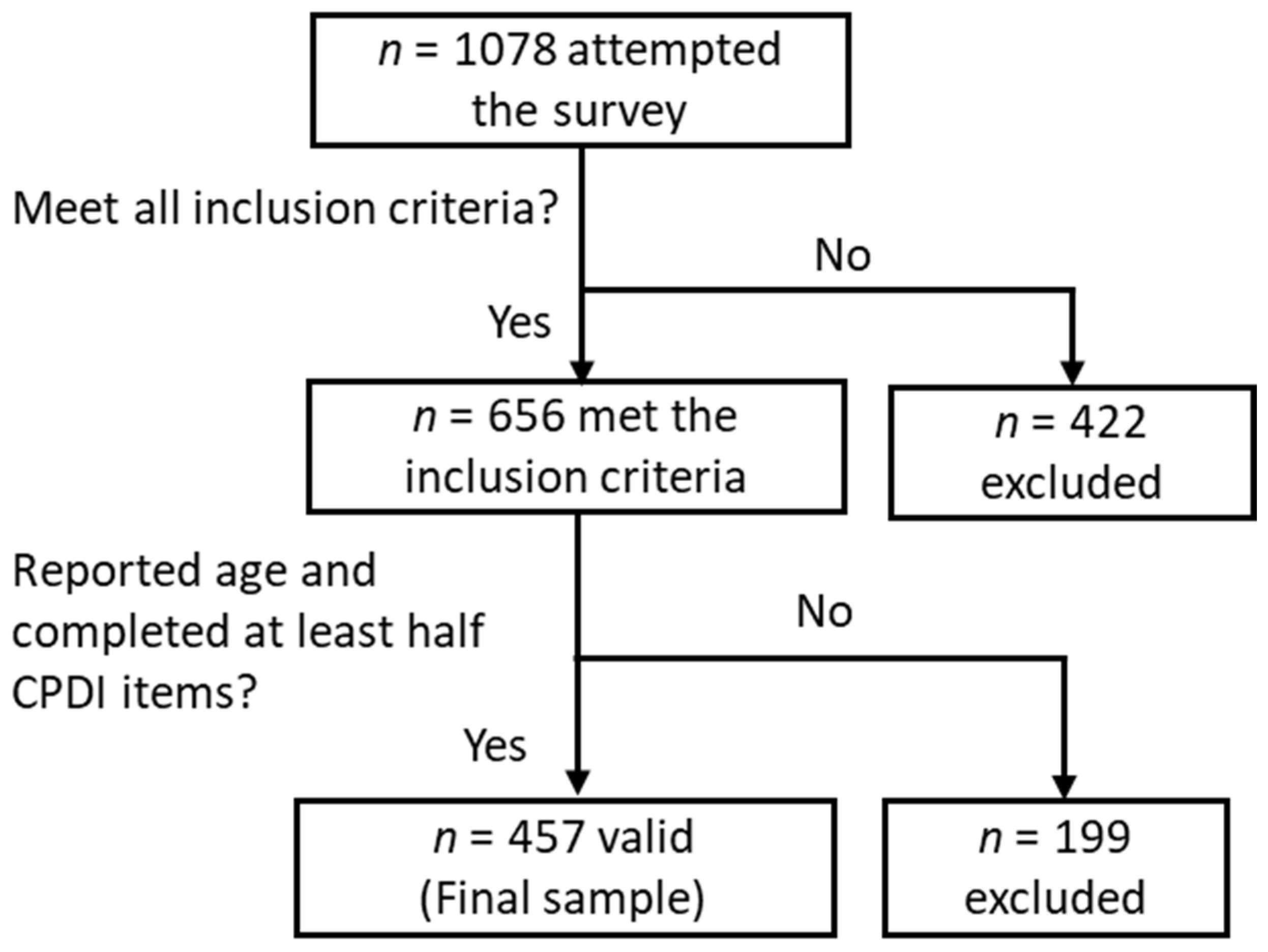
Figure 1.
Sample selection procedure (n = 457).
Figure 1.
Sample selection procedure (n = 457).
Table 1.
Sample characteristics and their group differences in CPDI (n = 457).
Table 1.
Sample characteristics and their group differences in CPDI (n = 457).
| Variables | n (%) | CPDI | |||
|---|---|---|---|---|---|
| M (SD) | F | p | |||
| Age group | <35 | 43 (9.41) | 21.53 (11.29) | 3.46 | 0.032 |
| 35–64 | 361 (78.99) | 26.80 (14.33) | |||
| ≥65 | 53 (11.60) | 20.83 (11.51) | |||
| Sex | Female | 330 (72.21) | 26.50 (14.09) | 1.00 | 0.319 |
| Male | 123 (26.91) | 23.40 (13.43) | |||
| Years in Canada | 0–5 years | 70 (15.32) | 23.80 (13.22) | 1.00 | 0.368 |
| 6–15 years | 159 (34.79) | 27.21 (14.96) | |||
| >15 years | 225 (49.23) | 25.19 (13.37) | |||
| Marital status | Married/Partnered | 378 (82.71) | 25.63 (13.71) | 0.06 | 0.803 |
| Other | 79 (17.29) | 25.52 (15.08) | |||
| Education | College and under | 108 (23.63) | 28.26 (15.06) | 3.62 | 0.058 |
| University and above | 348 (76.15) | 24.85 (13.47) | |||
| Employment status | Employed | 209 (45.73) | 26.51 (14.18) | 2.87 | 0.036 |
| Self-employed | 90 (19.69) | 24.79 (12.29) | |||
| Retired/Student | 92 (20.13) | 21.64 (12.58) | |||
| Unemployed/Other | 66 (14.44) | 29.42 (15.87) | |||
| Housing type | Owed | 361 (78.99) | 25.73 (14.10) | 1.70 | 0.193 |
| Other | 96 (21.01) | 25.17 (13.39) | |||
| Housing size | 1–2 people | 119 (26.04) | 25.35 (14.98) | 3.05 | 0.048 |
| 3–4 people | 248 (54.27) | 26.80 (13.50) | |||
| 5 or more people | 83 (18.16) | 22.68 (13.64) | |||
| Region | Ontario | 373 (81.62) | 26.35 (13.98) | 8.28 | 0.004 |
| Other provinces | 84 (18.38) | 22.33 (13.39) | |||
| Religion | No | 246 (53.83) | 26.14 (14.48) | 2.47 | 0.086 |
| Christianity/Catholicism | 131 (28.67) | 24.24 (11.75) | |||
| Other | 80 (17.51) | 26.20 (15.52) | |||
| Coping behaviour endorsement | Exercise (Yes/No) | 300 (65.65)/157 (34.35) | 24.31 (12.87)/28.09 (15.54) | 2.65 | 0.104 |
| Reading (Yes/No) | 243 (53.17)/214 (46.83) | 24.20 (12.92)/27.21 (14.89) | 4.49 | 0.035 | |
| Lis. music (Yes/No) | 230 (50.33)/227 (49.67) | 24.56 (13.98)/26.67 (13.86) | 0.01 | 0.931 | |
| Drinking tea (Yes/No) | 119 (26.04)/338 (73.96) | 25.22 (13.47)/25.75 (14.12) | 0.42 | 0.519 | |
| Chatting (Yes/No) | 249 (54.49)/208 (45.51) | 24.67 (13.04)/26.73 (14.91) | 0.29 | 0.593 | |
| Music Coping | Class. music (Yes/No) | 196 (42.89)/261 (57.11) | 24.87 (13.36)/26.17 (14.37) | 0.39 | 0.532 |
| Nature music (Yes/No) | 238 (52.08)/219 (47.92) | 25.90 (13.62)/25.29 (14.32) | 0.16 | 0.691 | |
| Pop music (Yes/No) | 158 (34.57)/299 (65.43) | 23.87 (13.32)/26.53 (14.20) | 2.06 | 0.152 | |
| Relig. music (Yes/No) | 100 (21.88)/357 (78.12) | 25.07 (14.32)/23.68 (13.62) | 0.07 | 0.792 | |
| Love song (Yes/No) | 96 (21.01)/361 (78.99) | 23.68 (13.63)/26.12 (14.00) | 1.98 | 0.160 | |
Table 2.
Linear regression of the sociodemographic predictors of the CPDI (n = 448).
Table 2.
Linear regression of the sociodemographic predictors of the CPDI (n = 448).
| Step | Predictors | CPDI | ||||
|---|---|---|---|---|---|---|
| β | 95% CI | R2 | F | |||
| 1 | SWLS | −1.21 *** | −1.40, −1.02 | 0.28 | 33.89 *** | |
| Coping: Exercise | Yes (reference) No/missing |
1.27 | −1.13, 3.66 | |||
| Coping: Reading | Yes (reference) No/missing |
1.05 | −1.21, 3.32 | |||
| Coping: Pop music | Yes (reference) No/missing |
2.24 | −0.12, 4.60 | |||
| Coping: Love song | Yes (reference) No/missing |
0.76 | −1.98, 3.51 | |||
| 2 | SWLS | −0.49 *** | −0.71, −0.27 | 0.45 | 18.58 *** | |
| Coping: Exercise | Yes (reference) No/missing |
0.30 | −1.88, 2.47 | |||
| Coping: Reading | Yes (reference) No/missing |
1.24 | −0.83, 3.30 | |||
| Coping: Pop music | Yes (reference) No/missing |
0.76 | −1.39, 2.91 | |||
| Coping: Love song | Yes (reference) No/missing |
−0.06 | −2.53, 2.42 | |||
| Age group | <35 (reference) | |||||
| 35–64 | 4.19 * | 0.40, 7.98 | ||||
| ≥65 | 2.20 | −2.96, 7.35 | ||||
| Education | College/under (reference) | |||||
| University and above | −1.67 | −4.23, 0.89 | ||||
| Employment | Employed (reference) | |||||
| status | Self-employed | −2.03 | −4.73, 0.67 | |||
| Retired/student | −4.68 * | −8.41, −0.96 | ||||
| Unemployed/other | −0.21 | −3.33, 2.91 | ||||
| Housing type | Owed (reference) | |||||
| Other | 1.55 | −1.20, 4.30 | ||||
| Housing size | 1–2 people (reference) | |||||
| 3–4 people | 0.21 | −2.28, 2.70 | ||||
| 5 or more people | −2.93 | −6.04, 0.18 | ||||
| Region | Ontario (reference) | |||||
| Other provinces | −3.02 * | −5.76, −0.29 | ||||
| Religion | No (reference) | |||||
| Christianity/Catholicism | −2.06 | −4.41, 0.30 | ||||
| Other | −1.15 | −4.02, 1.72 | ||||
| Family income | 1 = lowest, 5 = highest | 0.37 | −0.73, 1.47 | |||
| Health status | 1 = very poor, 5 = very good | −7.95 ** | −9.59, −6.32 | |||
Table 3.
COVID-related group differences in the CPDI (N = 457).
Table 3.
COVID-related group differences in the CPDI (N = 457).
| Variables | N (%) | CPDI | |||
|---|---|---|---|---|---|
| M (SD) | F | p | |||
| COVID-19 Experience | Infection/exposure status Yes No/missing |
43 (9.41) 414 (90.59) |
29.09 (15.81) 25.25 (13.71) |
3.50 | 0.062 |
| Action status Yes No/missing |
54 (11.82) 403 (88.18) |
22.62 (12.05) 26.01 (14.14) |
3.52 | 0.061 | |
| COVID-19 Behaviour | Avoidance behaviour Yes No/missing |
451 (98.69) 6 (1.31) |
25.73 (13.94) 16.53 (11.90) |
1.98 | 0.160 |
| Endorsement behaviour Yes No/missing |
448 (98.03) 9 (1.97) |
25.72 (13.97) 20.02 (11.89) |
0.23 | 0.629 | |
Table 4.
Correlations between continuous predictors and the CPDI.
Table 4.
Correlations between continuous predictors and the CPDI.
| Variables | M (SD) | CPDI | ||
|---|---|---|---|---|
| r | p (2-Tailed) | |||
| Sociodemographic | ||||
| Family income | 1 = lowest, 5 = highest | 2.94 (1.02) | −0.104 | 0.027 |
| Health status | 1 = very poor, 5 = very good | 3.58 (0.80) | −0.618 | 0.000 |
| COVID-19 Cognition | ||||
| Infection likeliness | 1 = lowest, 5 = highest | 3.11 (0.90) | 0.194 | 0.000 |
| Self-contraction worry | 1 = lowest, 5 = highest | 3.50 (1.04) | 0.423 | 0.000 |
| Family-contraction worry | 1 = lowest, 5 = highest | 3.83 (1.03) | 0.341 | 0.000 |
| Information authenticity concern | 1 = lowest, 5 = highest | 2.95 (0.95) | 0.263 | 0.000 |
| Canada measure attitude | 1 = very positive, 5 = very negative | 2.51 (1.18) | 0.189 | 0.000 |
| Threat perception | 1 = lowest, 5 = highest | 4.21 (0.80) | 0.255 | 0.000 |
| Discrimination perception | 1 = lowest, 5 = highest | 3.54 (0.97) | 0.299 | 0.000 |
| Future infection prediction | 0–100% | 19.86 (16.38) | 0.220 | 0.000 |
| Personal behavioural measure perception | 1 = completely ineffective, 5 = completely effective |
4.05 (0.57) | 0.061 | 0.195 |
| Personal health hygiene perception | 1 = completely ineffective, 5 = completely effective |
3.36 (0.95) | 0.137 | 0.004 |
| Public measure Support | 1 = firmly oppose, 5 = firmly support | 4.42 (0.54) | −0.022 | 0.637 |
| Moderators | ||||
| SWLS | 1 = strongly disagree, 7 = strongly agree | 24.73 (5.79) | −0.515 | 0.000 |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
[ad_2]