Healthcare | Free Full-Text | Considering Burnout and Well-Being: Emergency Medicine Resident Shift Scheduling Platform and Satisfaction Insights from a Quality Improvement Project
1. Introduction
2. Methods
2.1. Needs Assessment
As a needs assessment, we conducted an anonymous Google Form baseline satisfaction survey of our upper-level residents (n = 32) posted in our residency SMS group chat in May of 2023. This survey had four components. First, we asked residents to rate their satisfaction with schedules made by outgoing chief residents during the 2022–2023 academic residency year on a Likert scale from 1 (strongly unsatisfied) to 5 (strongly satisfied). Second, residents were also given a free response section to list pain points with the 2022–2023 schedules. Third, in the same baseline survey, residents were asked to rate their satisfaction with the June 2023 schedule created by the incoming chief residents and, fourth, asked to provide free response pain points with the June 2023 schedule. Excluding the December schedule, for which we have different holiday scheduling rules, follow-up surveys were sent to residents at two month increments to track satisfaction for the August and October 2023 schedules. Residents were sent reminders to complete the surveys via the same SMS group chat, and the response rate for the baseline survey served as the target response rate for subsequent surveys. Our baseline needs assessment survey had a response rate of 7/32 (22%). Response rates for the August and October surveys were 7/32 (22%) and 9/32 (28%), respectively.
2.2. Study Design
2.3. Data Analysis
We examined relationships of satisfaction with scheduling software/platforms/characteristics using Mann–Whitney U tests. Manual scheduling, scheduling practice length <2 years, and programs with ≤30 residents served as the references. Relationships between scheduler and scheduler-perceived resident satisfaction were evaluated using Spearman correlations. Survey questions without answers were coded as “Unknown.” All statistical analyses were performed using R Version 4.2.2 (R Core Team, Vienna, Austria) and a p-value < 0.05 was used as the threshold for statistical significance.
3. Results
Our external survey response rate was estimated at 19/253 (8%). Twelve surveys (63%) were completed by program directors, four (21%) were completed by assistant/associate program directors, one (5%) was completed by a chief resident, one (5%) was completed by a program coordinator, and one (5%) person did not specify their program role. The responses represented all United States regions (i.e., northeast, southeast, midwest, west, and southwest). Ten programs (53%) were responsible for regularly scheduling more than thirty residents. Only two programs (11%) reported scheduling manually without any special software. Of the manually scheduled programs, one did not report their program size, while the other reported scheduling for less than 30 residents. ShiftAdmin was the most popular scheduling software used (53% of respondents).
Free-response questions demonstrated software cost, long-term program use, and the same platform used for faculty/attending scheduling as the primary reasons for which the programs decided to use a specific software platform. Common pain points included suboptimal automation algorithms given the complexity of scheduling even after meeting with software representatives, steep learning curves that new chief residents must learn each year, and cost. Respondents also pointed to residency program features such as chronic understaffing, scheduling residents at multiple sites, scheduling residents of different training levels, and unlimited resident day-off requests as factors that further complicated the scheduling process.
4. Discussion
In this quality improvement project and convenience sample pilot survey, we examined the relationships of scheduling platforms/characteristics with scheduler and scheduler-perceived resident satisfaction. The results from our internal needs assessment demonstrated that residents became more satisfied with chief resident schedules over time. Our external survey demonstrated that manual scheduling was consistently ranked the poorest in terms of scheduler-perceived resident satisfaction and was among the bottom-ranked platforms in terms of scheduler satisfaction. We also observed higher scheduler-perceived resident and scheduler satisfaction in programs incorporating scheduling software, programs with thirty or less residents, and programs using their scheduling platform for more than two years.
While we do have residency program representation from each United States region, our study is limited by its small sample size. Our external survey aimed to address ways of improving the continued administrative burden of schedule-making, but was limited by a poor survey response rate (8%). Only two programs reported strictly manual scheduling, and there were no statistically significant findings related to satisfaction and scheduling platforms/characteristics. Still, we believe that the results remain informative as a pilot study and the only emergency medicine study of its kind that we could identify through a literature review. Furthermore, we recognize the need for more comprehensive research in this area and hope that our pilot study can help inform these efforts. Finally, our external survey relied on the perceptions of residency leaders responding to the survey and no resident non-schedulers were surveyed. Directly surveying resident non-schedulers in all survey instruments will be critical in future work. In addition to utilizing larger sample sizes, future studies may also benefit from more comprehensive analyses of scheduling software platform features and an evaluation of long-term impacts of scheduling practices.
5. Conclusions
In summary, we report findings of scheduler and scheduler-perceived resident satisfaction with emergency medicine resident scheduling platforms and characteristics. Although not statistically significant, these latter data suggest that existing scheduling software needs to be improved and that there may be resident and scheduler benefits to using scheduling software. Ultimately, our work can help to inform more comprehensive studies as well as efforts aimed at tackling physician wellness by optimizing scheduling practices.
Author Contributions
J.C.N.-E. and J.N.S. conceived and designed the study. J.C.N.-E. performed the data analyses and drafted the manuscript. T.F.E., B.G., H.M., A.C., M.S., B.A.W. and M.G. contributed to the analyses. All authors have read and agreed to the published version of the manuscript.
Funding
This study received no external funding.
Institutional Review Board Statement
This project met the criteria for non-human subject research based on the Emory University Institutional Review Board determination form.
Informed Consent Statement
Not applicable.
Data Availability Statement
Data are contained within the article.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Lin, M.; Battaglioli, N.; Melamed, M.; Mott, S.E.; Chung, A.S.; Robinson, D.W. High Prevalence of Burnout Among US Emergency Medicine Residents: Results From the 2017 National Emergency Medicine Wellness Survey. Ann. Emerg. Med. 2019, 74, 682–690. [Google Scholar] [CrossRef]
- World Health Organization. Burn-Out an “Occupational Phenomenon”: International Classification of Diseases. Available online: https://www.who.int/news/item/28-05-2019-burn-out-an-occupational-phenomenon-international-classification-of-diseases (accessed on 16 October 2023).
- Williamson, K.; Lank, P.M.; Cheema, N.; Hartman, N.; Lovell, E.O. Comparing the Maslach Burnout Inventory to Other Well-Being Instruments in Emergency Medicine Residents. J. Grad. Med. Educ. 2018, 10, 532–536. [Google Scholar] [CrossRef] [PubMed]
- Soares, J.P.; Lopes, R.H.; de Souza Mendonça, P.B.; Silva, C.R.D.V.; Rodrigues, C.C.F.M.; de Castro, J.L. Use of the Maslach Burnout Inventory Among Public Health Care Professionals: Scoping Review. JMIR Ment. Health 2023, 10, e44195. [Google Scholar] [CrossRef] [PubMed]
- Rischall, M.L.; Chung, A.S.; Tabatabai, R.; Doty, C.; Hart, D. Emergency Medicine Resident Shift Work Preferences: A Comparison of Resident Scheduling Preferences and Recommended Schedule Design for Shift Workers. AEM Educ. Train. 2018, 2, 229–235. [Google Scholar] [CrossRef]
- Stowell, J.R.; Vohra, T.T.; Luber, S.D. Emergency Medicine Resident Clinical Hours: A National Survey. J. Emerg. Med. 2015, 48, 474–480.e4. [Google Scholar] [CrossRef]
- Jeanmonod, R.; Jeanmonod, D.; Ngiam, R. Resident Productivity: Does Shift Length Matter? Am. J. Emerg. Med. 2008, 26, 789–791. [Google Scholar] [CrossRef] [PubMed]
- Steele, M.T.; Ma, O.J.; Watson, W.A.; Thomas, H.A. Emergency Medicine Residents’ Shiftwork Tolerance and Preference. Acad. Emerg. Med. 2000, 7, 670–673. [Google Scholar] [CrossRef] [PubMed]
- Stehman, C.R.; Testo, Z.; Gershaw, R.S.; Kellogg, A.R. Burnout, Drop Out, Suicide: Physician Loss in Emergency Medicine, Part I. West. J. Emerg. Med. 2019, 20, 485–494. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Mu, M.; He, Y.; Cai, Z.; Li, Z. Burnout in Emergency Medicine Physicians. Medicine 2020, 99, e21462. [Google Scholar] [CrossRef] [PubMed]
- Hafner, J.W.; Gardner, J.C.; Boston, W.S.; Aldag, J.C. The Chief Resident Role in Emergency Medicine Residency Programs. West. J. Emerg. Med. 2010, 11, 120–125. [Google Scholar] [PubMed]
- Chenais, G.; Lagarde, E.; Gil-Jardiné, C. Artificial Intelligence in Emergency Medicine: Viewpoint of Current Applications and Foreseeable Opportunities and Challenges. J. Med. Internet Res. 2023, 25, e40031. [Google Scholar] [CrossRef] [PubMed]
Figure 1.
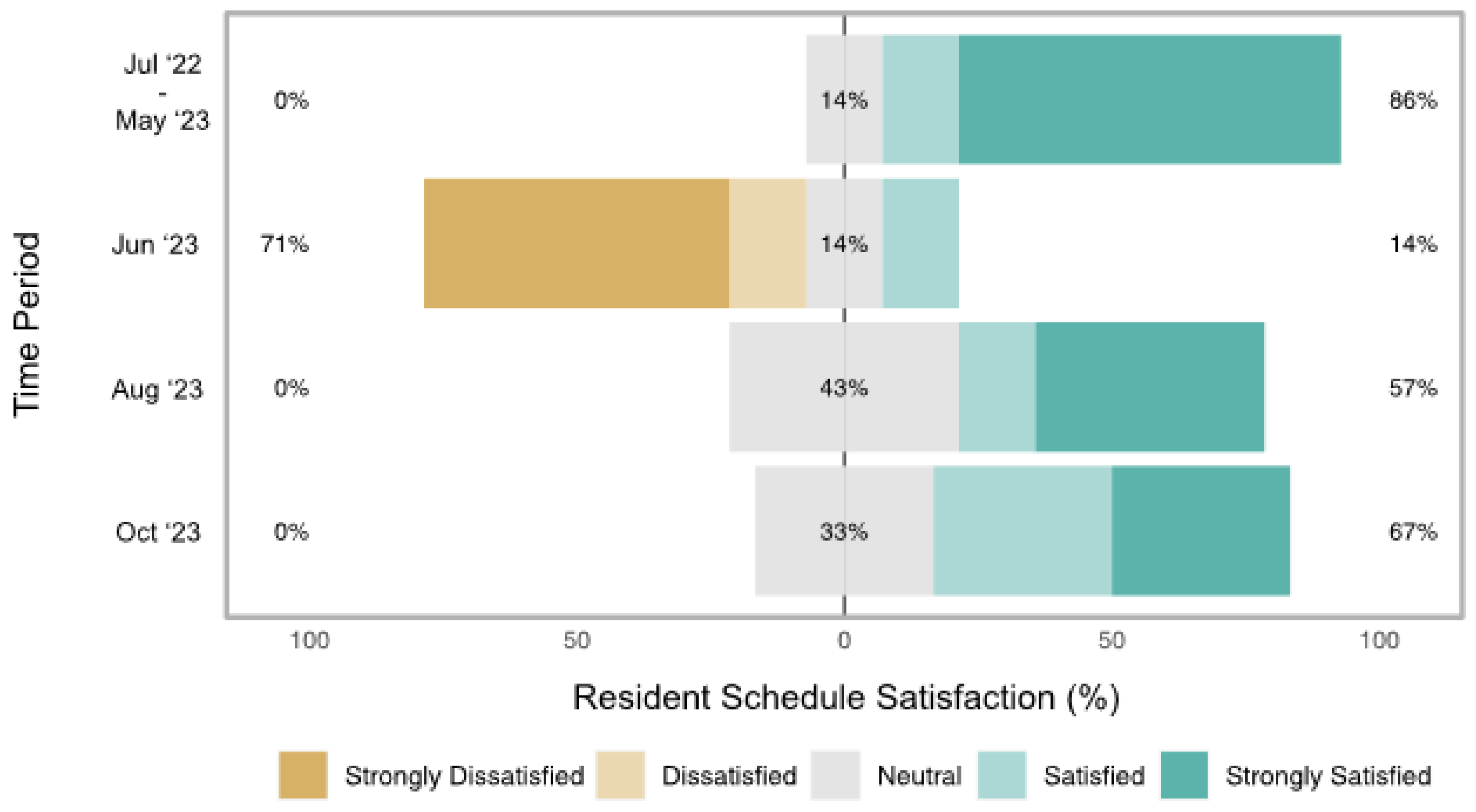
Resident reported schedule satisfaction from the needs assessment survey. This figure presents a centered horizontal bar plot of internal program resident schedule satisfaction throughout the quality improvement study period. June 2023 satisfaction (the first schedule made by new chief residents) was significantly lower (p = 0.01) than academic year July 2022–May 2023 satisfaction (schedules made by old chief residents). Subsequent schedules created by the new chief residents achieved greater resident satisfaction, as August 2023 (p = 0.02) and October 2023 (p = 0.01) resident satisfaction was statistically greater than baseline June 2023 resident satisfaction. There was no statistically significant difference in resident satisfaction in August 2023 (p = 0.28) and October 2023 (p = 0.23) compared to academic year July 2022–May 2023, suggesting that new chiefs achieved satisfaction levels comparable to the old chiefs. p-Values from Mann–Whitney U tests.
Figure 1.
Resident reported schedule satisfaction from the needs assessment survey. This figure presents a centered horizontal bar plot of internal program resident schedule satisfaction throughout the quality improvement study period. June 2023 satisfaction (the first schedule made by new chief residents) was significantly lower (p = 0.01) than academic year July 2022–May 2023 satisfaction (schedules made by old chief residents). Subsequent schedules created by the new chief residents achieved greater resident satisfaction, as August 2023 (p = 0.02) and October 2023 (p = 0.01) resident satisfaction was statistically greater than baseline June 2023 resident satisfaction. There was no statistically significant difference in resident satisfaction in August 2023 (p = 0.28) and October 2023 (p = 0.23) compared to academic year July 2022–May 2023, suggesting that new chiefs achieved satisfaction levels comparable to the old chiefs. p-Values from Mann–Whitney U tests.
Table 1.
Pain-point comments from the internal resident satisfaction needs assessment survey free responses.
Table 1.
Pain-point comments from the internal resident satisfaction needs assessment survey free responses.
| Easy to get burnt out if you have several evening shifts in a row. |
| Difficult to transition to overnight shifts with no calendar day off in between the day shift and night shift. |
| Wellness can be compromised when you have to go directly from an off service rotation into the next rotation (I’m sure this is out of your control though). |
| When prior chiefs made schedules, they considered shifts surrounding requests off. This schedule does not do that (i.e., trying to leave for a weekend and I got it off but I work 3–11 on Friday and work backup Monday making travel very difficult). |
| Would prefer multiple days in a row and having extended 3 days off in a row. |
| Would prefer longer stretches of shifts with longer stretches of days off rather than multiple strings of just 2–3 shifts with one day off in between, but that may just be personal preference. |
| Wish I had more grouped breaks and not just one day off at a time. |
| It’s a little brutal to have 2 sets of night shifts on split adult and pediatric months. I’m not sure if there’s a work around or a way to create balance between our schedules. |
| Finished overnights at the end of September and then switched back to nights again 1st week of October. |
Table 2.
External national ACGME-accredited schedule satisfaction survey content.
Table 2.
External national ACGME-accredited schedule satisfaction survey content.
|
|
|
1 (least) = Strongly Unsatisfied. 5 (most) = Strongly Satisfied |
1 (least) = Strongly Unsatisfied. 5 (most) = Strongly Satisfied |
|
|
|
Table 3.
Relationships of schedule platforms and characteristics with scheduler and scheduler-perceived resident satisfaction from an external pilot survey.
Table 3.
Relationships of schedule platforms and characteristics with scheduler and scheduler-perceived resident satisfaction from an external pilot survey.
| Scheduler Satisfaction Mean (Median) |
p-Value | Scheduler-Perceived Resident Satisfaction Mean (Median) |
p-Value | |
|---|---|---|---|---|
| Overall | ||||
| Study Sample (n = 19) | 3.4 (3) | – | 3.2 (3) | – |
| Scheduling Platform | ||||
| Manual (n = 2) | 3 (3) | reference | 2.5 (2.5) | reference |
| MedRez (n = 2) | 3 (3) | 0.99 | 3.5 (3.5) | 0.67 |
| MetricAid (n = 1) | 4 (4) | 0.99 | 4 (4) | 0.99 |
| Qgenda (n = 3) | 2.3 (3) | 0.99 | 3 (3) | 0.99 |
| ShiftAdmin (n = 10) | 3.7 (3.5) | 0.82 | 3.3 (3) | 0.73 |
| Qgenda/ShiftAdmin (n = 1) | 4 (4) | 0.99 | 4 (4) | 0.99 |
| Scheduling Format | ||||
| Manual (n = 2) | 3 (3) | reference | 2.5 (2.5) | reference |
| Software (n = 16) | 3.3 (3) | 0.99 | 3.3 (3) | 0.66 |
| Unknown (n = 1) | 5 (5) | 0.99 | 5 (5) | 0.67 |
| Scheduling Practice Length | ||||
| <2 years (n = 4) | 2.8 (3) | reference | 2.8 (3) | reference |
| 2–4 years (n = 7) | 3.3 (3) | 0.63 | 3.7 (4) | 0.28 |
| 4–6 years (n = 3) | 3.3 (3) | 0.69 | 3.3 (4) | 0.58 |
| >6 years (n = 5) | 4 (4) | 0.20 | 3 (3) | 0.79 |
| Number of Residents | ||||
| ≤30 (n = 4) | 3.75 (3.5) | reference | 4 (4) | reference |
| >30 (n = 10) | 3.2 (3) | 0.50 | 3.4 (3.5) | 0.25 |
| Unknown (n = 5) | 3.4 (3) | – | 2.4 (2) | – |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |