IJERPH | Free Full-Text | Improving Adolescent Psychosocial Assessment through Standardized Patient Simulation: An Interdisciplinary Quality Improvement Initiative
1. Introduction
The aims of this interdisciplinary QI project were to enhance the physician and nursing residents’ interviewing processes with their adolescent patients and to improve the identification of modifiable risk outcomes within this specific pediatric tertiary care center. The purpose of this interdisciplinary QI project was to pilot an SP program based on the HEEADSSS interviewing process within the physician and nursing residencies of a pediatric tertiary care center, and to improve the early identification of modifiable risk factors of suicidality among adolescent patients.
2. Materials and Methods
2.1. Design
2.2. Sample
The project was reviewed by an Institutional Review Board and was determined to not meet the definition of research involving human subjects. Additional measures to protect the rights and confidentiality of both resident participants and SPs included a confidentiality and video consent agreement and an opt-out clause, without explanation, for any simulated scenario that made the SP or resident uncomfortable.
2.3. Instrumentation
2.4. Procedures
To prepare resident participants for their scheduled session, prerequisite education was emailed one week preceding the event with instructions to review prior to their arrival at the session. The 45 min self-study module included links to a one-page HEEADSSS guide with examples of open-ended questions, a PowerPoint detailing laws and guidelines for adolescent confidentiality in Texas, a model adolescent psychosocial interview video demonstration, and a short article regarding conducting a HEEADSSS assessment in 15 min.
Here is a brief overview of the flow of the QI pilot program: 1. Participants are briefed upon arrival and are assigned as pairs (such as a nurse–physician pair). 2. These pairs are assigned to an exam room with a standardized-patient-adolescent–guardian duo to conduct a full psychosocial interview. 3. These pairs are provided a copy of their individual results and reconvene for a forty-minute group reflection guided by the LCSW. 4. These pairs are then assigned to a second exam room with another SP-adolescent–guardian duo to conduct a second full psychosocial interview. 5. These pairs are next provided a copy of their individual results and reconvene for another forty-minute group reflection guided by the LCSW. The following paragraph gives more information on the flow of the pilot program.
Participants were briefed upon arrival at the simulation center to establish psychological safety and expectations for the encounter. The sample group of 36 physician residents and nursing residents was then divided into nurse–physician pairs, or if no nurse was available, a physician intern in their first year was paired with a senior physician resident. Each member of the pair was assigned two fictitious patients and provided a brief history of present illness for review prior to entering the exam room.
Participants were randomly assigned to an exam room where an adolescent–guardian SP duo awaited them. The fictitious patient “Taylor,” portrayed simultaneously by all three SP adolescents, was the first on the schedule. The physician or nursing resident assigned to that patient was allotted ten minutes to conduct a full psychosocial interview using any resources necessary while the second resident observed. Following the ten-minute interview, SPs were given three minutes to individually evaluate the encounter and seven minutes to engage in constructive verbal feedback utilizing the SCAG as a guide. Guardian SPs allowed the adolescent SPs to guide the debrief and supplemented when appropriate. After the individual debrief, the process was repeated for the second resident in the pair with the next fictitious patient on the schedule, “Jaime”.
Following the initial encounter, all three physician–nurse or physician–physician-resident pairs were provided a copy of their individual SCAG results and reconvened as a large group in the simulation classroom for a forty-minute group reflection guided by the LCSW. To maximize resources and provide ample opportunity for participation, during this time, the second group of six residents initiated their initial interviews.
After a group guided reflection, the physician–nurse or physician–physician-resident pairs were escorted to new exam rooms where a different set of SPs awaited them. The interview and debrief processes were repeated with the next two fictitious patients on the schedule, “Chris” and “Kelly”. This follow-up strategy was utilized to preserve the sense of unfamiliarity one might feel meeting an adolescent patient for the first time. After their two-hour simulation activity, each physician or nursing resident had directly performed two and observed two adolescent psychosocial interviews with SP feedback for a total of four encounters.
2.5. Analysis
Data collection commenced with the baseline survey to gather demographics, preliminary SE-12 scores, and current use of HEEADSSS in clinical practice. Response options regarding the current utilization of HEEADSSS in practice were based on a five-point Likert scale (1 = Never, 2 = Rarely, 3 = Occasionally, 4 = Frequently, and 5 = Almost Always). Subsequent SE-12 surveys were administered immediately following the activity and again four weeks after the completion of all simulation sessions. The four-week follow-up survey also asked participants to self-report using the HEEADSSS assessment in clinical practice. All surveys were distributed utilizing Qualtrics XM (Silver Lake, Menlo Park, CA, USA) experience management software. Additionally, adolescent and guardian SPs evaluated residents’ performance in the initial and subsequent interviews on a copy of the SCAG, which was later transcribed to a spreadsheet. Finally, reports of social work referrals from 1 August 2021 to 22 May 2022 were obtained from the organization’s decision support team.
Individual scores and responses were matched via the participants’ unique identification numbers and analyzed utilizing JASP 0.18.2 (Amsterdam, Netherlands) statistical software. Participants’ initial and follow-up total-item scores were aggregated, and a one-tailed paired t-test was performed to establish the existence of a positive change in performance for both SE-12 and SCAG scores. Results for HEEADSSS use in practice were codified where 1 = never or rarely, 2 = occasionally, and 3 = Frequently or Almost Always, and a Wilcoxon signed-rank test was used to determine significant changes in clinical use.
Social work referrals were filtered by the provider type, patient age, chief complaint, and referral reason to quantify the weekly rate of mental or behavioral health-related referrals to the social work department for adolescent patients (11–21 years) presenting with a non-mental-health-related chief complaint. The mean number of weekly referrals was analyzed utilizing a control chart. The upper and lower control limits were determined using baseline data prior to the week of implementation. The remaining weekly data following implementation were plotted on the control chart and analyzed for any special cause patterns or shifts in the center line.
3. Results
Significant improvements were noted in this QI pilot. These included improved confidence in clinical communication, improved clinical competence in performing comprehensive psychosocial interviews, improvements in the early identification of modifiable risk factors of suicidality among adolescent patients, and an increase in the number of social work referrals related to modifiable risk factors for patients presenting with a non-mental-health-related chief complaint following the last simulation session.
Self-confidence in adolescent communication improved by 13%. These results immediately following the SP simulation showed (M = 8.45), t (35) = −4.29, and p ≤ 0.001 and at four-week follow-up, (M = 8.64), t (10) = −5.94, and p ≤ 0.001 as compared to baseline (M = 7.68). For the clinical competence in performing comprehensive psychosocial interviews, the pre- and post-SCAG results revealed improvements in participants’ performance of the SCAG 33-item checklist from the initial (M = 50.42) to the follow-up interview (M = 55.83), t (35) = −3.37, and p ≤ 0.001, and an overall 11% increase in self-efficacy in communicating with adolescents from baseline. Each SCAG section did have the option to assign a global score (A, B, C, D, F); however, this was not completed consistently and thus was not utilized in the analysis. Additionally, improvements in the early identification of modifiable risk factors of suicidality among adolescent patients were demonstrated by the incidence of residents self-reporting the use of HEEADSSS in clinical practice, as either Frequently or Almost Always designations increased from 47% at baseline to 64% at four-week follow-up. A Wilcoxon Signed-Rank Test indicated a significant mean rank change from baseline (M = 2.16) to follow-up (M = 2.55), p = 0.02.
4. Discussion
This SP interviewing simulation QI pilot demonstrates various strengths and implications for clinical assessment of adolescent mental health issues. Standard patient simulations, such as the one utilized in this QI clinical education project, can effectively enhance nursing preparation and practice by delivering a more seamless transition in the development of competencies for nursing residents, especially when accompanied by the inclusion of patient care interactions with other interdisciplinary team members. Notably, SP programs, especially those using interprofessional collaboration, can be utilized by all healthcare disciplines to develop and refine motivational interviewing skills, enhance providers’ practice of collaboratively managing difficult behaviors, and culturally prepare providers for successfully engaging in challenging or problematic conversations. This is particularly relevant in increasing various healthcare providers’ competency developments in their communications and interactions with at-risk adolescents.
This interdisciplinary SP interviewing simulation QI pilot was beneficial in improving the 36 nursing and physician residents’ ability to conduct psychosocial assessments for risk factors of suicidality among adolescents. An increased transfer of knowledge was noted through the enhancement of the nursing and physician providers’ confidence and competence within this project’s simulation lab, as the concept of adoption corresponded to the increased reported use of HEEADSSS in practice, and the outcomes were directly related to the number of adolescents identified who could benefit from additional social work support. This is notable that by improving the effective communication skills of the nursing and physician residents, a more thorough screening was performed to ensure that those at-risk adolescents who might benefit from a social work consult would receive it in an efficient and timely manner. This SP simulation QI pilot will be a valuable addition to both the nursing and physician residency programs, especially since much of the cost associated with the planning, design, and development of the curriculum has already been completed. Moving forward, the next phase in this QI plan will be to integrate the adolescent SP psychosocial interprofessional collaborative assessment activity into the academic schedule to coincide with residents’ adolescent and developmental health rotations.
Our community’s youth are experiencing a mental health crisis, culminating in rising adolescent suicide rates. An early identification of modifiable risk factors can help adolescents receive the support they need to successfully navigate this vulnerable stage of growth and development. An early identification of those modifiable risk factors could also potentially decrease the number of suicide rates among this age group, especially among the female adolescent population who are most at risk.
While this QI pilot had many strengths, there were some limitations. One of the limitations was the inability to accurately measure social work requests originating from nursing as all screenings are documented under the admitting physician. An additional limitation was that no formal measure was established to consider the effects of the interdisciplinary aspect of the activity, although one nursing participant stated “This is so helpful to hear how the doctors interact with the patients and what types of questions they ask”. Additional limitations were that there was a potential for biases in self-report measures for the increases in confidence and self-efficacy, and as this was a pilot program, there was no control group or comparison with other training methods, or with traditional training approaches regarding effectiveness and efficiency. The authors acknowledge that the lack of a control group contributes to the limited referential nature of the findings and conclusions in this QI pilot project.
5. Conclusions
Subsequent to the adolescent SP simulations, confidence in clinical communication skills of the nursing and physician residents increased by 13%, clinical competency in performing comprehensive psychosocial interviews increased by 11%, use of HEEADSSS increased by 64%, and social work referrals increased by 89%. Although many pediatric healthcare providers voice a lack in confidence in their ability to interact effectively with adolescents, the literature supports the use of adolescent SP simulation as an educational modality to improve clinicians’ interactions with adolescents. The result of this QI pilot indicates the strength of this recommendation as well. With the current emphasis on improving nursing education’s assessment and evaluation methods through the enhancement in teaching modalities, especially those incorporating interprofessional education, simulation, and collaboration, this QI pilot exhibits advancements within these associated realms.
In the future, the adolescent SP interviewing simulations will become a routine course of the interdisciplinary interactions offered by this pediatric tertiary care center’s simulation center. The success of this QI pilot warrants an ongoing re-evaluation of this particular organization’s previously siloed educational model to assess whether additional opportunities for incorporating and encouraging interprofessional education to promote the mutual appreciation of interdisciplinary collaboration can be further achieved. Thus, other healthcare providers and disciplines will be invited to take part in this program to help them consider how SP methodology can be used to improve the quality of care offered in their designated specialty areas.
Additionally, aside from the positive interprofessional collaborative developments exhibited in this experience itself, participants’ use of written resources to guide the adolescent interview processes had improved their performance significantly. Currently, there are no specific cues within the EMR for the HEEADSSS framework, which may indicate another opportunity for future improvements. Due to the intricacies of Texas confidentiality laws, this will require close collaboration with the health records, ethics, and compliance offices to ensure positive outcomes for healthcare providers, patients, and guardians. The development of closer collaborative efforts evidenced through this project can augment those continuing developments to achieve these results.
The results of this QI pilot manifested positive steps in the enhancement in the training of the nursing and physician resident interprofessional teams and increased their educational initiatives for collaborative competencies and interactions. This pilot demonstrated improvements in the interdisciplinary healthcare providers’ practices to assess, identify, and intervene in their points of contact with at-risk adolescents. These confidence and competency improvements demonstrated by this QI pilot for nursing and physician residents to conduct adolescents’ psychosocial assessments for risk factors of suicidality can further enhance adolescents’ ongoing care. It is a win/win outcome for all.
Author Contributions
Conceptualization, C.L.E. and L.M. (Laura Monahan); methodology, C.L.E. and L.M. (Laura Monahan); formal analysis, C.L.E. and L.M. (Laura Monahan); investigation, C.L.E., J.F., L.M. (Lisa McKenna) and E.E.-I.; resources, C.L.E. and L.M. (Laura Monahan); data curation, C.L.E.; writing—original draft preparation, C.L.E., L.M. (Laura Monahan) and J.C.W.; writing—review and editing, C.L.E. and L.M. (Laura Monahan); visualization, C.L.E. and L.M. (Laura Monahan); supervision, C.L.E. and L.M. (Laura Monahan); project administration, C.L.E., E.E.-I., J.F., L.M. (Lisa McKenna) and L.M. (Laura Monahan). All authors have read and agreed to the published version of the manuscript.
Funding
This QI project received no external funding.
Institutional Review Board Statement
This project was reviewed by an Institutional Review Board and was determined to not meet the definition of research involving human subjects. The study was conducted in accordance with the Declaration of Helsinki and approved by the Institutional Review Board of Texas A&M University—Corpus Christi (TAMU-CC-IRB-2021-0318, date of approval: 17 November 2021).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the QI study.
Data Availability Statement
Data are available on request due to restrictions, e.g., privacy.
Acknowledgments
The authors wish to acknowledge support given by Julie Pina, MSN, RN, CNOR(E), NEA-BC, Chief Nursing Officer of Driscoll Health System.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- American Academy of Pediatrics (AAP). AAP-AACAP-CHA Declaration of a National Emergency in Child and Adolescent mental Health. 2021. Available online: https://www.aap.org/en/advocacy/child-and-adolescent-healthy-mental-development/aap-aacap-cha-declaration-of-a-national-emergency-in-child-and-adolescent-mental-health/ (accessed on 20 December 2023).
- Ivey-Stephenson, A.; Demissie, Z.; Crosby, A.; Stone, D.; Gaylor, E.; Wilkins, N.; Lowry, R.; Brown, M. Suicidal ideation and behaviors among high school students—Youth risk behavior Survey, 2019. Morb. Mortal. Wkly. Rep. Suppl. 2020, 69 (Suppl. S1), 47–55. [Google Scholar] [CrossRef] [PubMed]
- Yard, E.; Radhakrishnan, L.; Ballesteros, M.F. Emergency department visits for suspected suicide attempts among persons aged 12–25 years before and during the COVID-19 pandemic—United States, January 2019–May 2021. Morb. Mortal. Wkly. Rep. 2021, 70, 888–894. [Google Scholar] [CrossRef] [PubMed]
- Shepard, D.S.; Gurewich, D.; Lwin, A.K.; Reed, G.A., Jr.; Silverman, M.M. Suicide and suicidal attempts in the United States: Costs and policy implications. Suicide Life-Threat. Behav. 2016, 46, 352–362. [Google Scholar] [CrossRef] [PubMed]
- Doran, C.; Kinchin, I. Economic and epidemiological impact of youth suicide in countries with the highest human development index. PLoS ONE 2020, 14, 347. [Google Scholar] [CrossRef] [PubMed]
- Bilsen, J. Suicide and youth: Risk factors. Front. Psychiatry 2018, 9, 540. [Google Scholar] [CrossRef] [PubMed]
- Horowitz, L.; Tipton, M.V.; Pao, M. Primary and secondary prevention of youth suicide. Pediatrics 2020, 145 (Suppl. S2), S195–S203. [Google Scholar] [CrossRef] [PubMed]
- Fallucco, E.M.; Hanson, M.D.; Glowinski, A.L. Teaching pediatric residents to assess adolescent suicide risk with a standardized patient module. Pediatrics 2010, 125, 953–959. [Google Scholar] [CrossRef]
- Tanski, S.; Garfunkel, L.C.; Duncan, P.M.; Weitzman, M. Performing Preventive Services: A Bright Futures Handbook, 1st ed.; American Academy of Pediatrics: Itasca, IL, USA, 2020; ISBN 10:1581105223. [Google Scholar]
- Goldenring, J.M.; Cohen, E. Getting into adolescent heads. Contemp. Pediatr. 1988, 5, 75–90. Available online: https://www.contemporarypediatrics.com/view/getting-adolescent-heads (accessed on 1 December 2021).
- Borzutzky, C. Adolescent medicine and pediatric residency training: The value of collaboration and shared educational resources. J. Adolesc. Health Off. Publ. Soc. Adolesc. Med. 2021, 68, 842–843. [Google Scholar] [CrossRef]
- National Research Council; Institute of Medicine Committee on Adolescent Health Care Services and Models of Care for Treatment, Prevention, and Healthy Development. Summary findings and overall conclusions. In Adolescent Health Services: Missing Opportunities; Lawrence, R.S., Appleton Gootman, J., Sim, L.J., Eds.; National Academies Press (US): Washington, DC, USA, 2009; pp. 296–310. Available online: https://www.ncbi.nlm.nih.gov/books/NBK215418/ (accessed on 20 December 2023).
- Sawyer, S.M.; Conn, J.J.; Reid, K.J.; Dodds, A.E.; Hudson, L.; Yeo, M.; Proimos, J. Working with young people: Evaluation of an education resource for medical trainees. J. Paediatr. Child Health 2013, 49, 901–905. [Google Scholar] [CrossRef]
- Spitznagle, J.; Balmuri, N.; Adams, A.; Onel, K.; Taber, S.; Pan, N. Identifying targets to improve the assessment of psychosocial risk factors in adolescent patients: Perspectives from pediatric rheumatology fellows in the United States and Canada. In Arthritis Rheumatology; Wiley: Hoboken, NJ, USA, 2020; Volume 72, Available online: https://acrabstracts.org/abstract/identifying-targets-to-improve-the-assessment-of-psychosocial-risk-factors-in-adolescent-patients-perspectives-from-pediatric-rheumatology-fellows-in-the-united-states-and-canada/ (accessed on 5 December 2021).
- Gamble, A.; Bearman, M.; Nestel, D. A systematic review: Children & adolescents as standardized patients in health professional education. Adv. Simul. 2016, 1, 1. [Google Scholar] [CrossRef]
- Lioce, L.; Lopreiato, J.; Downing, D.; Chang, T.P.; Robertson, J.M.; Anderson, M.; Diaz, D.A.; Spain, A.E. The Terminology and Concepts Working Group. Healthcare Simulation Dictionary, 2nd ed.; Lioce, L., Lopreiato, J., Spain, A.E., Eds.; AHRQ Publication No. 20-0019; Agency for Healthcare Research and Quality: Rockville, MD, USA, 2020. [Google Scholar] [CrossRef]
- Joukhadar, N.; Bourget, G.; Manos, S.; Mann, K.; Hatchette, J.; Blake, K. Skills for interviewing adolescent patients: Sustainability of structured feedback in undergraduate education on performance in residency. J. Grad. Med. Educ. 2016, 8, 422–425. [Google Scholar] [CrossRef] [PubMed]
- Luebbert, R.; Popkess, A. The influence of teaching method on performance of suicide assessment in baccalaureate nursing students. J. Am. Psychiatr. Nurses Assoc. 2015, 21, 126–133. [Google Scholar] [CrossRef] [PubMed]
- Logan, J.; Graham, I.D. Toward a comprehensive interdisciplinary model of health care research use. Sci. Commun. 1998, 20, 227–246. [Google Scholar] [CrossRef]
- Axboe, M.K.; Christensen, K.S.; Kofoed, P.; Ammentorp, J. Development and validation of a self-efficacy questionnaire (SE-12) measuring the clinical communication skills of health care professionals. BMC Med. Educ. 2016, 16, 272. [Google Scholar] [CrossRef] [PubMed]
- Dogbey, G. Critical synthesis package: Structured communication adolescent guide (SCAG). J. Teach. Learn. Resour. 2014, 10, 9690. [Google Scholar] [CrossRef]
- Blake, K.; Mann, K.; Kutcher, M. The structured communication adolescent guide (SCAG). J. Teach. Learn. Resour. 2008, 4, 798. [Google Scholar] [CrossRef]
- Lewis, K.L.; Bohnert, C.A.; Gammon, W.L.; Hölzer, H.; Lyman, L.; Smith, C.; Thompson, T.M.; Wallace, A.; Gliva-McConvey, G. The Association of Standardized Patient Educators (ASPE) Standards of Best Practice (SOBP). Adv. Simul. 2017, 2, 10. [Google Scholar] [CrossRef]
- Wolderslund, M.; Kofoed, P.; Ammentorp, J. The effectiveness of a person-centred communication skills training programme for the health care professionals of a large hospital in Denmark. Patient Educ. Couns. 2021, 104, 1423–1430. [Google Scholar] [CrossRef]
- Kaplonyi, J.; Bowles, K.A.; Nestel, D.; Kiegaldie, D.; Maloney, S.; Haines, T.; Williams, C. Understanding the impact of simulated patients on health care learners’ communication skills: A systematic review. Med. Educ. 2017, 51, 1209–1219. [Google Scholar] [CrossRef]
- Hayes, S.C.; Ciarrochi, J.; Hofmann, S.G.; Chin, F.; Sahdra, B. Evolving an idionomic approach to processes of change: Towards a unified personalized science of human improvement. Behav. Res. Ther. 2022, 156, 104155. [Google Scholar] [CrossRef]
- Wilbur, K.; Elmubark, A.; Shabana, S. Systematic review of standardized patient use in continuing medical education. J. Contin. Educ. Health Prof. 2018, 38, 3–10. [Google Scholar] [CrossRef]
- Lugo, R.G.; Hjelmeland, I.; Hansen, M.T.; Haug, E.; Sütterlin, S.; Grønlien, H.K. Impact of initial emotional states and self-efficacy changes on nursing students’ practical skills performance in simulation-based education. Nurs. Rep. 2021, 11, 267–278. [Google Scholar] [CrossRef]
- Slade, S.; Sergent, S.R. Interview techniques. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2021. Available online: https://www.ncbi.nlm.nih.gov/books/NBK526083/ (accessed on 20 December 2023).
- Martin, P.A.; Loughins, L.; Weatherup, N.; Mullen, S. Bridging the gap: Using interspecialty high-fidelity simulation to improve skills in adolescent emergency medicine. Pediatr. Emerg. Care 2021, 37, 621–623. [Google Scholar] [CrossRef]
- Zortea, T.C.; Cleare, S.; Wetherall, K.; Melson, A.J.; O’Connor, R.C. On suicide risk: From psychological processes to clinical assessment and intervention. In Reference Module in Neuroscience and Biobehavioral Psychology; Elsevier: Amsterdam, The Netherlands, 2021; Available online: https://www.sciencedirect.com/topics/medicine-and-dentistry/assessment-of-suicide-risk (accessed on 20 December 2023).
- Richardson, A.E.; Cooper, M.; Wood, D.M. Are we using the HEEADSSS assessment to screen for psychosocial risks when young people are admitted to hospital? Arch. Dis. Child. 2018, 103, A4. [Google Scholar] [CrossRef]
- Substance Abuse and Mental Health Services Administration. SAMHSA’s Concept of Trauma and Guidance for a Trauma-Informed Approach; HHS Publication No. (SMA); Substance Abuse and Mental Health Services Administration: Rockville, MD, USA, 2014; p. 14-4884. Available online: https://ncsacw.acf.hhs.gov/userfiles/files/SAMHSA_Trauma.pdf (accessed on 20 December 2023).
Figure 1.
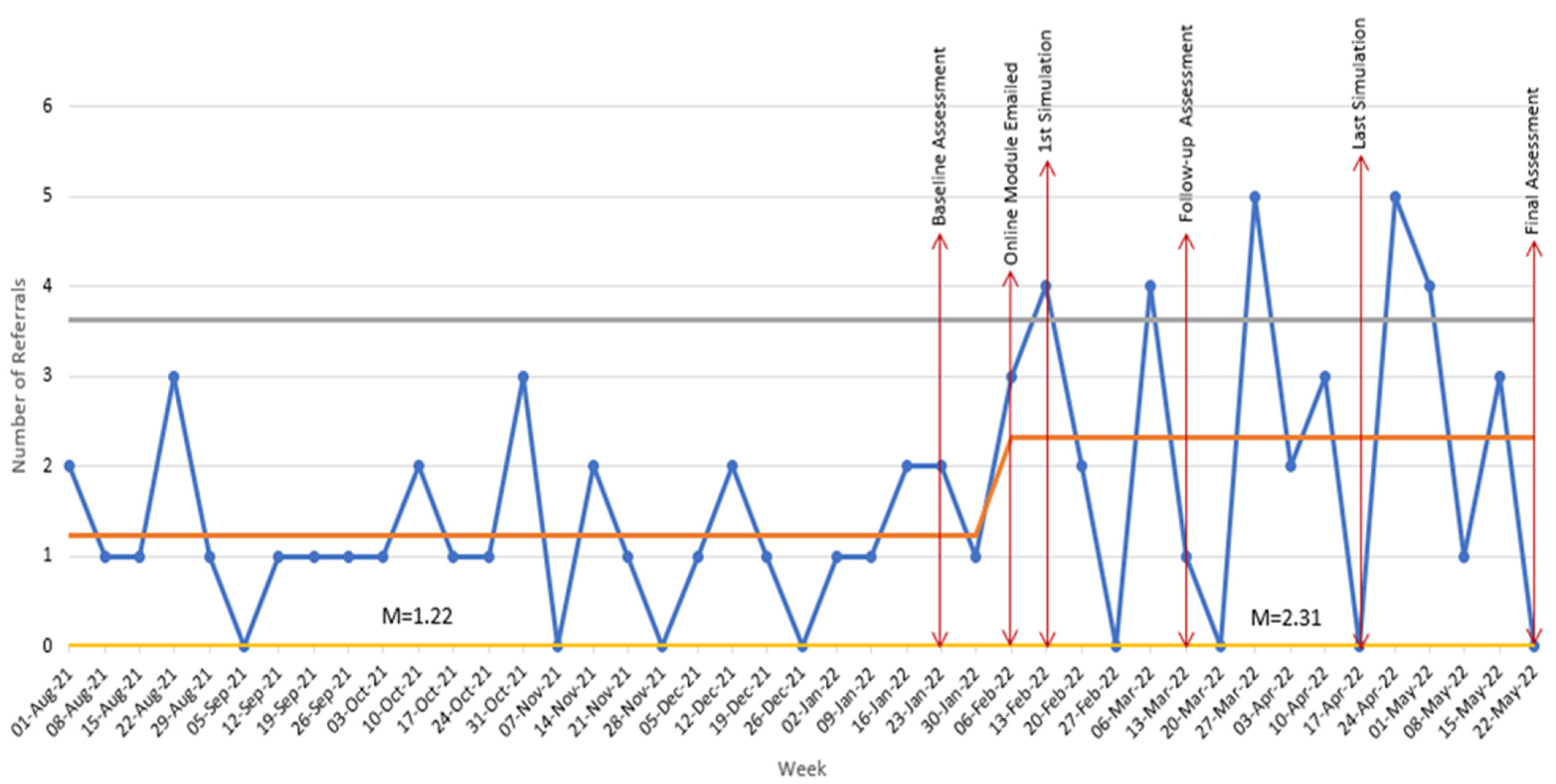
Weekly physician resident referrals to social work for adolescents presenting with non-mental or behavioral health primary diagnosis. The Yellow Line is the lower control limit of the number of psycho-social referrals to social work; The Orange Line is the mean average of the number of psycho-social referrals to social work; The Blue Line is the actual number of psycho-social referrals to social work; The Grey Line is the upper control limit of the number of psycho-social referrals to social work.
Figure 1.
Weekly physician resident referrals to social work for adolescents presenting with non-mental or behavioral health primary diagnosis. The Yellow Line is the lower control limit of the number of psycho-social referrals to social work; The Orange Line is the mean average of the number of psycho-social referrals to social work; The Blue Line is the actual number of psycho-social referrals to social work; The Grey Line is the upper control limit of the number of psycho-social referrals to social work.
Table 1.
Participants’ Demographics.
Table 1.
Participants’ Demographics.
| Physician | Nursing | Total | |
|---|---|---|---|
| Number of Residents | 22 | 14 | 36 |
| Age | |||
| Mean (SD) | 34.9 (6.7) | 27.3 (4.4) | 31.9 (7.0) |
| Gender | |||
| Female | 12 (55%) | 11 (79%) | 23 (64%) |
| Male | 10 (45%) | 3 (21%) | 13 (36%) |
| Ethnicity | |||
| Asian | 5 (23%) | 1 (7%) | 6 (17%) |
| Black or African American | 8 (36%) | 0 (0%) | 8 (22%) |
| Hispanic, Latino, or Spanish Origin | 5 (23%) | 7 (50%) | 12 (33%) |
| White | 3 (14%) | 2 (14%) | 5 (14%) |
| Two or More Ethnicities or Other | 1 (4%) | 4 (29%) | 5 (14%) |
| Education | |||
| Doctor of Medicine (MD) | 21 (95%) | ||
| Doctor of Osteopathic Medicine (DO) | 1 (5%) | ||
| Associate Degree in Nursing (ADN) | 9 (64%) | ||
| Bachelor of Science in Nursing (BSN) | 5 (36%) | ||
| Previous Yrs. of Healthcare Experience | |||
| None | 7 (32%) | 7 (50%) | 14 (39%) |
| 0–3 Years | 4 (18%) | 3 (21%) | 7 (19%) |
| 4–9 Years | 7 (32%) | 2 (14%) | 9 (25%) |
| 10+ Years | 4 (18%) | 2 (14%) | 6 (17%) |
| History of HEEADSSS Education | |||
| No | 6 (27%) | 8 (57%) | 14 (39%) |
| Unsure | 1 (5%) | 4 (29%) | 5 (14%) |
| Yes | 15 (68%) | 2 (14%) | 17 (47%) |
| Physician Post-Graduate Year | |||
| PGY-1 | 11 (50%) | ||
| PGY-2 | 7 (32%) | ||
| PGY-3 | 4 (18%) | ||
| Time in Nurse Residency | |||
| 0–2 Months | 8 (57%) | ||
| 3–5 Months | 3 (21%) | ||
| 6–8 Months | 3 (21%) |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |